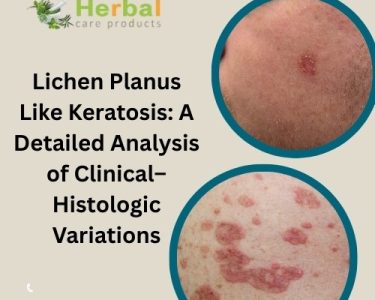
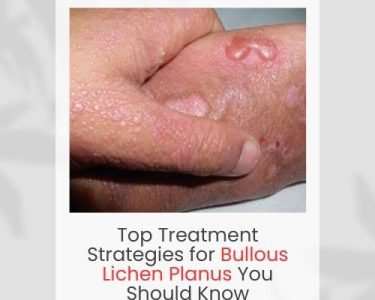
Lichen planus is a chronic inflammatory condition that affects the skin, mouth, scalp, nails, and sometimes the genitals. It is characterized by purple, itchy, flat-topped bumps on the skin and painful lesions in the mouth. While the condition has been recognized for many years, the exact lichen planus causes remain somewhat unclear. Researchers believe it is primarily related to an abnormal immune response where the body mistakenly attacks its own skin or mucous membrane cells.
Understanding the lichen planus triggers, risk factors, and immune mechanisms behind the condition can help patients better manage symptoms and reduce flare-ups. Various factors—including infections, medications, genetic susceptibility, and stress—may contribute to the development of this disease.
We will explores the major lichen planus causes, explains the role of the immune system in autoimmune lichen planus, and examines the relationship between medications, infections like hepatitis C, and the condition.
Understanding Lichen Planus
Before exploring the causes, it’s important to understand what lichen planus is and how it affects the body.
Lichen planus is considered an inflammatory and immune-mediated disease. It most commonly appears in adults between the ages of 30 and 60, although it can occur at any age. The condition can affect different parts of the body, including:
- Skin
- Oral cavity (oral lichen planus)
- Scalp (lichen planopilaris)
- Nails
- Genitals
Symptoms vary depending on the affected area but often include:
- Itchy purple or reddish bumps
- White patches in the mouth
- Painful sores
- Nail damage or ridging
- Hair loss when the scalp is involved
Because the disease can present in several forms, identifying the underlying lichen planus causes is essential for effective treatment and prevention.
The Role of the Immune System in Lichen Planus
One of the most widely accepted explanations for autoimmune lichen planus is that the immune system mistakenly targets healthy cells in the skin or mucous membranes.
Autoimmune Reaction
In autoimmune diseases, the body’s immune system attacks its own tissues. In lichen planus, T-cells, a type of white blood cell, become activated and target keratinocytes (skin cells).
This immune attack leads to:
- Inflammation
- Skin damage
- The characteristic rash and lesions
Scientists believe that certain environmental triggers activate this immune response in individuals who are genetically predisposed.
Inflammatory Pathways
When the immune system becomes activated, several inflammatory pathways are triggered. These include:
- Cytokine release
- T-cell activation
- Damage to the basal layer of the skin
These processes lead to the distinctive appearance of lichen planus lesions.
Because the condition involves immune system dysfunction, many experts classify it as an immune-mediated or autoimmune condition.
Major Lichen Planus Causes
Although no single cause explains every case, several factors are believed to contribute to the development of lichen planus.
1. Genetic Predisposition
Genetics may play a role in determining who develops lichen planus. While the disease is not strictly hereditary, people with certain genetic markers may have a higher risk.
Research suggests that individuals with a family history of autoimmune diseases may be more susceptible to immune-related skin conditions like lichen planus.
Genetic susceptibility alone is usually not enough to cause the disease, but it may increase vulnerability when combined with other triggers.
2. Viral Infections
One of the most studied associations in dermatology is between hepatitis C and lichen planus.
Hepatitis C and Lichen Planus
Multiple studies have found a higher prevalence of lichen planus among people infected with hepatitis C. While the exact mechanism is still being investigated, researchers believe the virus may trigger an abnormal immune response that leads to skin inflammation.
Possible explanations include:
- Immune system cross-reactivity
- Chronic viral stimulation of immune cells
- Inflammation caused by viral proteins
However, not all people with hepatitis C develop lichen planus, and not all patients with lichen planus have hepatitis C.
Other viral infections have also been explored as possible contributors, though the evidence is less conclusive.
3. Medications Causing Lichen Planus
Certain drugs can trigger a lichenoid drug reaction, which closely resembles classic lichen planus. These reactions occur when the immune system responds to medication by attacking skin cells.
Common Medications Causing Lichen Planus
Some drugs known to trigger lichen planus-like eruptions include:
- Blood pressure medications (beta-blockers, ACE inhibitors)
- Nonsteroidal anti-inflammatory drugs (NSAIDs)
- Antimalarial medications
- Certain antibiotics
- Gold compounds used for arthritis
- Diuretics
When medications are responsible, the condition may be referred to as drug-induced lichen planus.
Symptoms often improve after discontinuing the medication, although it may take several weeks or months for lesions to disappear.
4. Dental Materials and Allergic Reactions
In oral lichen planus, reactions to dental materials may play a role.
Some people develop lesions in response to materials such as:
- Amalgam fillings
- Metal dental restorations
- Dental adhesives
These reactions are thought to be delayed hypersensitivity reactions, where the immune system reacts to substances in the mouth.
Replacing problematic dental materials sometimes improves symptoms.
5. Stress and Psychological Factors
While stress does not directly cause lichen planus, it can worsen symptoms and trigger flare-ups.
Chronic stress affects the immune system and may increase inflammation in the body. Many patients report that their symptoms become worse during periods of emotional stress or anxiety.
Stress-related hormonal changes can influence immune activity and may contribute to disease progression.
6. Injury or Skin Trauma (Koebner Phenomenon)
Another known lichen planus trigger is skin injury.
This phenomenon, known as the Koebner phenomenon, occurs when lesions appear at the site of skin trauma.
Examples of triggering injuries include:
- Scratches
- Burns
- Surgical scars
- Insect bites
In individuals with lichen planus, these injuries may activate the immune response and cause new lesions to develop.
Lichen Planus Triggers
While the underlying immune dysfunction may already exist, specific environmental factors can trigger the disease or cause flare-ups.
Common Lichen Planus Triggers
Some frequently reported triggers include:
- Certain medications
- Viral infections
- Stress
- Dental materials
- Skin injuries
- Chemical exposure
Triggers vary widely among individuals. Identifying personal triggers can help patients manage the condition more effectively.
Risk Factors for Developing Lichen Planus
Several factors may increase the likelihood of developing lichen planus.
Age
The condition is most common in middle-aged adults, particularly between 30 and 60 years old.
Gender
Some studies suggest that women may be more likely to develop oral lichen planus, although the skin form affects both genders equally.
Existing Autoimmune Disorders
Individuals with other autoimmune diseases may have a higher risk. Conditions often associated with autoimmune activity include:
- Thyroid disease
- Vitiligo
- Alopecia areata
These associations support the theory that autoimmune lichen planus is linked to immune system dysregulation.
The Link Between Hepatitis C and Lichen Planus
The connection between hepatitis C and lichen planus is one of the most researched areas in dermatology.
In some regions, studies show that up to 20–30% of lichen planus patients may have hepatitis C infection.
Possible Mechanisms
Researchers propose several explanations:
- Viral proteins may trigger immune responses against skin cells.
- Chronic infection may stimulate persistent immune activation.
- Genetic factors may predispose individuals to both conditions.
Doctors sometimes recommend hepatitis C screening for patients diagnosed with lichen planus, particularly in regions where the virus is common.
Types of Lichen Planus and Their Causes
Different forms of the disease may have slightly different triggers.
Cutaneous Lichen Planus
This form affects the skin and produces purple, itchy bumps.
Possible causes include:
- Immune system dysfunction
- Viral infections
- Medication reactions
Oral Lichen Planus
Oral lichen planus affects the inside of the mouth and may cause:
- White lacy patches
- Painful sores
- Burning sensations
Possible causes include:
- Immune reactions
- Dental material sensitivity
- Viral infections
Lichen Planopilaris
This type affects the scalp and can lead to permanent hair loss. It is believed to result from an autoimmune attack on hair follicles.
How Doctors Identify the Cause
Because the exact lichen planus causes vary, doctors often conduct several tests to identify possible triggers.
Medical History
Doctors ask about:
- Medications
- Recent infections
- Family history
- Dental procedures
Skin Biopsy
A small sample of skin may be examined under a microscope to confirm the diagnosis.
Blood Tests
Blood tests may be used to detect:
- Hepatitis C infection
- Other underlying conditions
Identifying triggers helps guide treatment strategies.
Managing Triggers and Reducing Flare-Ups
Although lichen planus cannot always be prevented, managing triggers can reduce symptom severity.
Avoiding Trigger Medications
If a drug-induced reaction is suspected, doctors may recommend switching medications.
Managing Stress
Stress-reduction techniques such as meditation, exercise, and therapy may help reduce flare-ups.
Oral Care
For oral lichen planus, good dental hygiene and avoiding irritating foods may help manage symptoms.
Monitoring Viral Infections
Testing and treating infections such as hepatitis C may improve overall health and potentially reduce symptoms.
When to See a Doctor
People should seek medical attention if they experience:
- Persistent itchy rashes
- Painful mouth sores
- Nail changes
- Hair loss on the scalp
Early diagnosis can help prevent complications and improve quality of life.
Future Research on Lichen Planus Causes
Researchers continue to study the immune mechanisms behind lichen planus.
Areas of ongoing research include:
- Genetic susceptibility
- Immune signaling pathways
- Viral triggers
- Targeted immunotherapy
Improved understanding of these factors may lead to more effective treatments in the future.
Conclusion
The exact lichen planus causes remain complex and multifactorial. Most evidence suggests that the condition results from an abnormal immune response in which the body attacks its own skin or mucous membrane cells.
Several factors may contribute to this immune reaction, including lichen planus triggers such as medications, viral infections, stress, and skin injuries. The association between hepatitis C and lichen planus further supports the role of immune system activation in the disease.
Additionally, certain medications causing lichen planus can trigger drug-induced reactions that mimic the condition. Understanding these triggers and risk factors helps patients and healthcare providers manage symptoms more effectively.
While autoimmune lichen planus cannot always be prevented, identifying triggers, managing stress, and receiving appropriate medical care or if anyone taking supplements take it under supervision, By opting these strategies can significantly improve outcomes and quality of life.