Living with achalasia can feel like navigating a constant maze of dietary adjustments, medical appointments, and lifestyle tweaks. If you’ve been diagnosed with this rare esophageal disorder, you know that it affects not just your digestion but also your quality of life. Achalasia occurs when the lower esophageal sphincter (LES) fails to relax properly, preventing food and liquids from passing smoothly from the esophagus into the stomach. Over time, this can lead to difficulties swallowing, regurgitation, chest discomfort, and weight loss.
While medical interventions such as pneumatic dilation, Heller myotomy, or peroral endoscopic myotomy (POEM) can alleviate the physical blockage, managing living with achalasia on a daily basis involves a combination of dietary strategies, lifestyle adjustments, and proactive symptom management. This guide will provide practical, research-backed tips to help you improve your day-to-day experience.
Understanding Achalasia: The Foundation for Daily Management
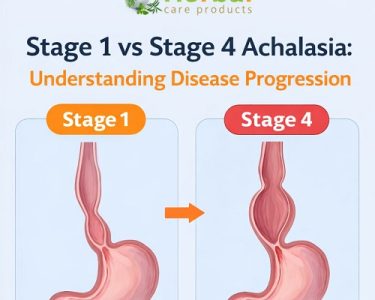
Before diving into daily management tips, it’s crucial to understand what happens in achalasia. The esophagus is a muscular tube that propels food from your mouth to your stomach using rhythmic contractions known as peristalsis. In achalasia, these contractions are impaired, and the LES remains unusually tight. This leads to:
- Dysphagia: Difficulty swallowing solids and sometimes liquids.
- Regurgitation: Undigested food or saliva may come back up, especially when lying down.
- Chest pain or pressure: Often mistaken for heartburn or cardiac issues.
- Weight loss and malnutrition: Due to reduced food intake.
Understanding these symptoms helps you tailor daily routines that minimize discomfort and maximize nutritional intake.
1. Dietary Adjustments for Living With Achalasia
Food management is arguably the most critical component of living with achalasia. Small, thoughtful changes can make mealtimes less stressful and more enjoyable.
a. Eat Smaller, More Frequent Meals
Instead of three large meals, aim for five to six smaller meals throughout the day. Smaller meals:
- Reduce the risk of food getting stuck in the esophagus.
- Make digestion easier, preventing discomfort and regurgitation.
b. Choose Softer, Easier-to-Swallow Foods
Soft and well-cooked foods tend to slide down more easily. Consider including:
- Mashed potatoes, rice, oatmeal, and pasta
- Soft-cooked vegetables like carrots, zucchini, or squash
- Ground meats or tender fish
- Yogurt, smoothies, and soups
Avoid tough meats, raw vegetables, and crusty breads unless you can adequately chew and moisten them.
c. Modify Food Texture
Blending, mashing, or pureeing foods can make swallowing safer and less painful. Some patients find that adding sauces or gravies helps food slide down more easily.
d. Chew Thoroughly and Eat Slowly
Chewing food into smaller pieces reduces the work your esophagus must do and decreases the risk of food getting stuck. Take your time—swallowing in a calm, relaxed state can make a noticeable difference.
e. Stay Hydrated with Meals
Taking small sips of water with meals can help push food into the stomach. However, avoid gulping large amounts, which may cause regurgitation or discomfort.
f. Identify Trigger Foods
Certain foods may worsen symptoms for some patients. Common culprits include:
- Very dry foods (crackers, toast)
- Highly acidic items (tomatoes, citrus fruits)
- Carbonated drinks
- Alcohol
Keeping a food diary can help pinpoint personal triggers.
2. Lifestyle Adjustments That Support Daily Comfort
Beyond diet, lifestyle habits play a significant role in living with achalasia. The following adjustments are practical ways to reduce symptoms day-to-day.
a. Maintain an Upright Position After Eating
Gravity helps food move through the esophagus. Experts recommend:
- Staying upright for 30–60 minutes after meals
- Avoiding lying down immediately after eating
Some people benefit from gently walking after meals, which encourages peristalsis.
b. Sleep With Your Head Elevated
Nighttime regurgitation is common in achalasia. Elevating your head while sleeping can prevent food from coming back up. Use:
- Adjustable bed frames
- Wedge pillows (30–45° incline)
This simple change can improve sleep quality and reduce nocturnal discomfort.
c. Avoid Tight Clothing
Clothing that compresses your abdomen can exacerbate reflux and chest discomfort. Opt for looser garments around the waist, especially after meals.
d. Manage Stress
Stress doesn’t cause achalasia, but it can worsen symptoms like chest pain or difficulty swallowing. Incorporate stress-reduction techniques such as:
- Deep breathing or meditation
- Gentle yoga or stretching
- Mindfulness exercises
e. Regular Physical Activity
Moderate exercise, like walking, swimming, or cycling, supports digestion and general health. Avoid vigorous activity immediately after meals, which may trigger regurgitation.
3. Medical and Therapeutic Strategies
While daily management focuses on diet and lifestyle, medical strategies play a complementary role in improving life with achalasia.
a. Regular Medical Follow-Ups
Living with achalasia requires ongoing monitoring. Your doctor may recommend:
- Periodic endoscopy to check for esophageal dilation or complications
- Manometry or imaging to evaluate esophageal function
Regular check-ins allow timely adjustments to your treatment plan.
b. Medication Management
Certain medications can help relax the LES or manage symptoms:
- Nitrates or calcium channel blockers may reduce LES pressure.
- Botulinum toxin (Botox) injections can temporarily relax the sphincter.
Medication effectiveness varies, and some patients may only need them short-term or as adjuncts to procedural treatments.
c. Understand Your Treatment Options
Procedures such as Heller myotomy, POEM, or pneumatic dilation are more definitive treatments for achalasia. While lifestyle adjustments remain essential, knowing your options helps you plan long-term symptom control.
d. Working With a Dietitian
A registered dietitian experienced in gastrointestinal disorders can help craft a nutrition plan that:
- Ensures adequate calorie and protein intake
- Adjusts textures to reduce dysphagia risk
- Identifies personal triggers and nutrient deficiencies
You can explore more about the disease of achalasia by visiting our product page.
4. Practical Tips for Eating Out
Social activities often revolve around meals, and eating out can be challenging when living with achalasia. Here are strategies to navigate restaurants:
a. Review Menus in Advance
Look for soft foods or dishes that can be modified. Soups, stews, mashed potatoes, and pasta are usually safe bets.
b. Ask for Modifications
Don’t hesitate to request softer cooking methods or sauces to help food slide down more easily. Restaurants are often accommodating.
c. Eat Slowly and Mindfully
Focus on each bite, chew thoroughly, and drink small sips between bites. Avoid rushing or multitasking while eating.
d. Bring Emergency Snacks
If you anticipate long waits or menu limitations, bring safe snacks like protein shakes or soft fruit to prevent hunger-related stress.
5. Emotional and Social Considerations
Living with achalasia affects more than just your physical health. Social interactions, emotional well-being, and mental health are equally important.
a. Join Support Groups
Connecting with others facing similar challenges can be incredibly validating. Support groups, both online and in-person, offer:
- Practical tips for symptom management
- Emotional support and encouragement
- Sharing experiences about procedures and treatments
b. Communicate Openly With Friends and Family
Explain your dietary needs and limitations. People are often more understanding than you might expect, and clear communication reduces stress in social settings.
c. Mind-Body Approaches
Mindfulness, meditation, and gentle yoga can improve overall well-being and reduce anxiety associated with eating or swallowing difficulties.
d. Counseling or Therapy
For some, coping with a chronic condition can lead to anxiety, depression, or social withdrawal. Professional counseling can help develop strategies for stress management and emotional resilience.
6. Managing Complications of Achalasia
Despite best efforts, complications can occur. Awareness and prompt management are crucial in living with achalasia.
a. Esophageal Dilation
Over time, achalasia can cause the esophagus to stretch or dilate, increasing regurgitation risk. Periodic imaging helps detect changes early.
b. Risk of Malnutrition
Difficulty swallowing may reduce calorie intake. Ensure you:
- Track your weight regularly
- Incorporate high-calorie, soft foods if necessary
- Consider oral nutritional supplements
c. Prevent Aspiration
Regurgitated food can enter the lungs, causing aspiration pneumonia. Tips to reduce risk include:
- Eating upright
- Avoiding eating right before bedtime
- Chewing thoroughly
d. Monitor for Esophageal Cancer
Chronic achalasia slightly increases the risk of esophageal cancer over decades. Discuss screening frequency with your gastroenterologist.
7. Technology and Tools to Support Daily Life
Modern technology can make living with achalasia more manageable.
a. Eating Aids
- Soft-tipped utensils for gentle chewing
- Thickening agents for beverages to reduce aspiration risk
- Portable water bottles to sip while eating
b. Health Apps
Tracking meals, symptoms, and hydration can reveal patterns and triggers, helping fine-tune daily management.
c. Meal Delivery Services
Services that offer pre-cooked, soft, or pureed meals can save time and reduce stress about cooking and swallowing safely.
8. Creating a Personalized Routine
The key to successful living with achalasia is personalization. Consider:
- Morning: Gentle stretching, hydration, small breakfast (soft foods)
- Midday: Small lunch, slow eating, brief walk afterward
- Afternoon: Snack if needed, stress-reduction techniques
- Evening: Light dinner, remain upright for 30–60 minutes, elevate head during sleep
Keeping consistent routines helps your body adapt and minimizes symptoms.
9. When to Seek Medical Attention
Even with careful management, certain symptoms require prompt attention:
- Severe chest pain or sudden swallowing difficulty
- Unintentional rapid weight loss
- Persistent vomiting or inability to keep fluids down
- Signs of aspiration, such as coughing or fever
Early intervention can prevent complications and improve long-term outcomes.
10. Key Takeaways for Living With Achalasia
Living with achalasia is a journey that combines medical care, lifestyle adaptation, dietary adjustments, and emotional support. Here’s a summary of practical strategies:
- Prioritize small, soft, well-chewed meals
- Stay upright after eating and elevate your head while sleeping
- Track and avoid trigger foods
- Incorporate stress management and gentle exercise
- Maintain regular medical follow-ups
- Seek support networks for emotional and social resilience
- Monitor for nutrition, weight changes, and complications
- Use technology and adaptive tools to make daily life easier
Remember, while achalasia is a chronic condition, it can be managed effectively. The combination of awareness, preparation, and professional guidance allows individuals to maintain a high quality of life, enjoy meals, and minimize discomfort.
Conclusion
Living with achalasia presents unique challenges, but with the right strategies, daily life can be manageable and fulfilling. By adopting thoughtful dietary habits, creating supportive routines, leveraging medical treatments, and maintaining emotional resilience, you can reduce symptoms and improve overall well-being. The key is consistency, personalization, and proactive care—empowering yourself to live comfortably despite the condition.
With careful planning, education, and support, thriving with achalasia is entirely possible.