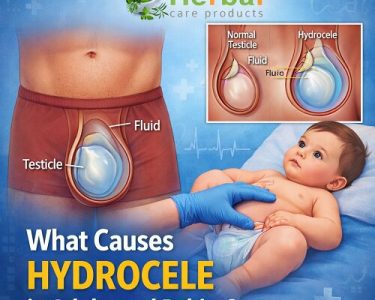
Hydrocele is a common medical condition characterized by the accumulation of fluid around the testicle, leading to swelling in the scrotum. While it is generally painless and often harmless, proper evaluation is essential to rule out underlying conditions such as infections, hernias, or, in rare cases, tumors. Understanding Hydrocele Diagnosis is crucial for timely management and reassurance.
What Is a Hydrocele?
A hydrocele occurs when fluid collects in the thin sheath surrounding the testicle. It can affect newborns, infants, and adult men. There are two main types:
- Communicating hydrocele: Linked to the abdominal cavity via an open channel.
- Non-communicating hydrocele: Fluid remains confined within the scrotum.
In adults, hydroceles may develop due to injury, infection, inflammation, or without any identifiable cause (idiopathic).
Why Accurate Hydrocele Diagnosis Matters
Although hydroceles are often benign, the symptoms can resemble other conditions that require medical attention. Proper Hydrocele Diagnosis helps to:
- Differentiate hydrocele from inguinal hernia
- Rule out testicular cancer
- Identify infections such as epididymitis
- Determine whether treatment is necessary
Early and accurate diagnosis ensures appropriate management and avoids unnecessary anxiety.
Initial Medical Consultation
The diagnostic process begins with a consultation. During this stage, the doctor gathers detailed information about the patient’s symptoms and medical history.
Medical History Assessment
Doctors typically ask questions such as:
- When did the swelling begin?
- Is the swelling painful or painless?
- Has the size changed over time?
- Is there any history of trauma or infection?
- Are there associated symptoms such as fever or urinary issues?
This information provides clues that guide further examination and testing.
Physical Examination
A thorough physical examination is the cornerstone of Hydrocele Diagnosis.
Inspection
The doctor visually examines the scrotum for:
- Swelling or enlargement
- Skin changes
- Symmetry between both sides
Hydroceles usually present as smooth, soft, and painless swelling.
Palpation
During palpation, the doctor gently feels the scrotum to assess:
- Size and consistency of the swelling
- Presence of tenderness
- Ability to feel the testicle separately
In a typical hydrocele, the swelling feels fluid-filled and the testicle may be difficult to palpate.
Transillumination Test
One of the simplest and most effective tools in Hydrocele Diagnosis is transillumination.
How It Works
- A bright light is placed behind the scrotum in a darkened room.
- If the swelling is filled with clear fluid, light passes through, producing a glowing effect.
Interpretation
- Positive transillumination: Suggests a hydrocele
- Negative transillumination: May indicate a solid mass, such as a tumor or hernia
While highly useful, this test is not definitive and is often followed by imaging studies.
Ultrasound Imaging
Importance of Ultrasound
Scrotal ultrasound is the gold standard in Hydrocele Diagnosis. It uses sound waves to create detailed images of the scrotal contents.
What Ultrasound Reveals
- Presence of fluid around the testicle
- Size and extent of the hydrocele
- Condition of the testicle and surrounding structures
- Detection of tumors, cysts, or infections
Advantages
- Non-invasive and painless
- Highly accurate
- No radiation exposure
Ultrasound is especially important when the diagnosis is uncertain or when complications are suspected.
Doppler Ultrasound
In some cases, doctors may use Doppler ultrasound to assess blood flow.
Why It’s Used
- To rule out testicular torsion (a medical emergency)
- To detect inflammation or infection
- To evaluate vascular abnormalities
This advanced imaging technique provides additional information that supports a precise diagnosis.
Laboratory Tests
Although not always necessary, lab tests may be ordered as part of Hydrocele Diagnosis when an underlying condition is suspected.
Blood Tests
- Check for signs of infection
- Evaluate inflammatory markers
Urine Tests
- Detect urinary tract infections
- Identify sexually transmitted infections
These tests help determine whether the hydrocele is secondary to another condition.
Differentiating Hydrocele from Other Conditions
One of the most critical aspects of Hydrocele Diagnosis is distinguishing it from other scrotal disorders.
Inguinal Hernia
- Occurs when part of the intestine protrudes into the scrotum
- Swelling may increase with coughing or straining
- Usually does not transilluminate
Varicocele
- Enlargement of veins in the scrotum
- Feels like a “bag of worms”
- More common on the left side
Epididymitis
- Inflammation of the epididymis
- Associated with pain, fever, and tenderness
Testicular Tumor
- Often presents as a firm, painless lump
- Does not transilluminate
- Requires urgent evaluation
Accurate differentiation ensures appropriate treatment and avoids misdiagnosis.
Special Considerations in Infants and Children
Hydroceles are common in newborns and usually resolve on their own.
Diagnostic Approach
- Physical examination is often sufficient
- Ultrasound may be used if diagnosis is unclear
Monitoring
Doctors typically monitor the condition for 6–12 months before considering intervention, as many cases resolve spontaneously.
When Additional Testing Is Needed
In some cases, further evaluation is required to confirm Hydrocele Diagnosis.
Indications for Additional Tests
- Rapid increase in size
- Severe pain
- Unclear diagnosis after initial assessment
- Suspicion of underlying pathology
Advanced imaging or specialist referral may be necessary in these situations.
Role of Specialists
Primary care physicians often initiate the diagnosis, but referral to a urologist may be needed.
When to See a Urologist
- Persistent or large hydroceles
- Uncertain diagnosis
- Associated complications
- Consideration of surgical treatment
Urologists have specialized expertise in managing scrotal conditions and ensuring accurate diagnosis.
Common Diagnostic Challenges
Despite straightforward methods, Hydrocele Diagnosis can sometimes be challenging.
Factors That Complicate Diagnosis
- Obesity or thick scrotal tissue
- Coexisting conditions
- Small or atypical hydroceles
In such cases, imaging becomes essential for clarity.
Importance of Early Diagnosis
Early detection of hydrocele ensures:
- Timely management
- Prevention of complications
- Peace of mind for the patient
While hydroceles are rarely dangerous, early evaluation helps rule out serious conditions.
Patient Preparation for Diagnosis
Patients can prepare for their medical visit by:
- Noting changes in swelling
- Reporting associated symptoms
- Providing medical history
- Being open about concerns
This helps doctors make an accurate and efficient diagnosis.
What Happens After Diagnosis?
Once Hydrocele Diagnosis is confirmed, the doctor determines the appropriate management plan.
Observation
- Small, asymptomatic hydroceles may not require treatment
- Regular monitoring is recommended
Medical Treatment
- Treat underlying infections if present
Surgical Intervention
- Hydrocelectomy for large or symptomatic hydroceles
- Aspiration (less commonly used)
The treatment decision depends on symptoms, size, and patient preference.
Frequently Asked Questions
Is Hydrocele Diagnosis Painful?
No, most diagnostic procedures are painless. Physical examination and ultrasound are non-invasive and comfortable.
Can Hydrocele Be Diagnosed at Home?
While swelling can be noticed at home, a proper medical evaluation is necessary for accurate diagnosis.
How Long Does Diagnosis Take?
In many cases, diagnosis can be made during a single visit, especially with access to ultrasound.
Conclusion
Hydrocele Diagnosis involves a systematic approach that includes medical history, physical examination, and imaging techniques. While the condition is often harmless, accurate diagnosis is essential to rule out more serious issues and ensure appropriate management.
From simple tests like transillumination to advanced imaging such as ultrasound, doctors use a range of tools to confirm the presence of a hydrocele. Understanding this process empowers patients to seek timely medical care and make informed decisions about their health.
If you notice any unusual swelling in the scrotum, consulting a healthcare professional is the best step toward accurate diagnosis and peace of mind.