Achalasia is a rare but often overlooked condition that affects the esophagus — the muscular tube that carries food from your mouth to your stomach. One question many people ask when learning about this disorder is: “Can achalasia cause weight loss?” The short answer is yes — achalasia can lead to significant weight loss, but the mechanisms are nuanced and go beyond just not being able to eat comfortably. We’ll explore exactly how achalasia contributes to weight loss, what symptoms accompany this process, how it’s diagnosed, and what options exist for treatment and nutritional recovery.
What Is Achalasia?
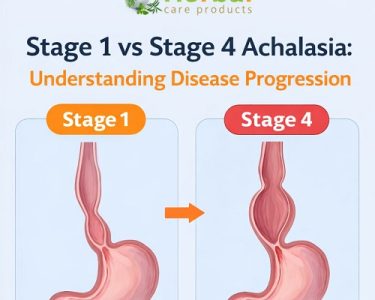
Achalasia is a swallowing disorder caused by nerve damage in the esophagus. Specifically, the lower esophageal sphincter (LES) — a muscular ring at the bottom of the esophagus — fails to relax properly. This malfunction prevents food and liquids from entering the stomach easily. At the same time, the coordinated muscle contractions that push food down (peristalsis) are weakened or lost.
Under normal conditions, the LES relaxes with each swallow to allow food to pass into the stomach. In achalasia, however, the LES remains too tight or doesn’t relax at all, and the esophagus lacks effective muscle activity, causing a functional obstruction. The food then pools in the esophagus instead of progressing into the digestive tract.
This is a chronic condition — it does not simply go away on its own. Although treatment can significantly improve symptoms, there is currently no cure.
Common Symptoms of Achalasia
Before diving into how achalasia leads to weight loss, it’s essential to recognize the symptoms that often precede or accompany the condition:
- Difficulty swallowing (dysphagia) — feels like food gets stuck in the throat or chest.
- Regurgitation — undigested food or saliva comes back up.
- Chest pain or discomfort — especially after eating.
- Heartburn, burping, or hiccups.
- Coughing or choking, particularly at night.
- Weight loss and malnutrition — see next sections.
Weight loss is often not listed first but becomes one of the most clinically significant results of the disease, particularly as symptoms advance.
How Achalasia Leads to Weight Loss
1. Difficulty Swallowing and Reduced Intake
The most direct way achalasia causes weight loss is by making it harder to eat enough food. Because swallowing feels uncomfortable or even painful, people tend to:
- Eat less food overall.
- Avoid large or solid meals.
- Prefer softer or liquid foods that don’t pass easily but are slightly more tolerable.
Difficulty swallowing translates to a reduced calorie intake, which over time results in a calorie deficit — the body loses weight because it’s using more energy than it’s consuming. In many patients with achalasia, the severity of dysphagia correlates strongly with weight loss patterns.
2. Regurgitation and Food Loss
Food that can’t make it to the stomach often comes back up as regurgitation or vomiting. Some patients may eat enough calories initially but end up regurgitating much of it before digestion can occur, which leads to poor nutrient absorption. Frequent regurgitation also discourages eating over time, further reducing caloric intake.
3. Lower Calorie and Nutrient Absorption
Physically, achalasia doesn’t directly block nutrient absorption, but because food may not reach the stomach consistently, the gut doesn’t receive sufficient nutrients. When caloric intake is chronically low, the body begins to use stored energy (fat and muscle) — a process that results in weight loss and eventual malnutrition in severe cases.
4. Severity and Subtypes Matter
Not all achalasia patients lose weight equally. Some studies indicate that patients with different forms of achalasia have varying risks of weight loss. For example, type II achalasia patients are more likely to lose significant weight than those with type III.
This suggests that the pattern of muscle and nerve dysfunction can influence how much the condition affects eating and nutritional status.
5. Psychological and Behavioral Factors
Chronic swallowing difficulties may also create food anxiety, where eating becomes a stressful experience. This can lead to intentional food avoidance, further contributing to weight loss. While this is not a direct physiological effect, it is a meaningful factor in many patients’ eating patterns.
How Common Is Weight Loss in Achalasia?
Weight loss doesn’t occur in every single person with achalasia, but it is very frequent. Research studies report that:
- Up to 57% of patients experience weight loss.
- Some older studies suggest that 31–80% of achalasia patients lose weight of varying degrees.
It’s worth noting that not all weight loss is severe, and some people may lose only a modest amount. In others, weight loss can be substantial — sometimes exceeding 20–40 pounds (9–18 kg) over months or years.
However, there are exceptions. Some people with achalasia do not lose weight, or their weight loss is mild. This often depends on how pronounced their swallowing difficulties are and how much dietary adaptation they develop over time.
Can Achalasia Cause Malnutrition?
Yes — when weight loss is chronic and severe, it often leads to malnutrition. This isn’t just about body weight — it’s also about body composition and nutrient balance. Patients may experience:
- Fatigue and weakness.
- Muscle wasting.
- Vitamin and mineral deficiencies.
- Immune suppression.
Research shows that achalasia patients are at nutritional risk regardless of their initial body mass index (BMI). Even people who start out overweight can become malnourished if achalasia prevents adequate intake.
Does Treatment Reverse Achalasia Weight Loss?
Yes — effective treatment often leads to weight gain and improved nutritional status.
Common therapies for achalasia include:
- Balloon dilation — to stretch the LES and improve passage of food.
- Surgical myotomy (e.g., Heller myotomy) — cutting the LES muscle to reduce obstruction.
- Peroral Endoscopic Myotomy (POEM) — a minimally invasive endoscopic incision of the LES.
These treatments help food pass more easily into the stomach, which restores caloric intake and often leads to weight stabilization and weight gain after treatment. Many studies show improved BMI and nutritional markers after successful therapy.
In fact, one study found that almost half the patients gained significant weight after treatment — and some became overweight — highlighting the dramatic shift in nutritional balance.
Other Health Impacts Related to Weight Loss
Weight loss in achalasia isn’t just about body size — it can have broader health implications:
1. Immunity & Healing
Malnutrition weakens the immune system, which makes infections more likely and can impair overall health.
2. Muscle and Strength Loss
Prolonged weight loss often involves loss of muscle as well as fat, reducing physical strength and endurance.
3. Quality of Life
Persistent discomfort with eating can lead to social and psychological challenges, including anxiety and depression.
4. Complications
Severe weight loss paired with regurgitation increases the risk of aspiration (food entering the lungs), which can cause pneumonia.
Diagnosis: How Is Achalasia Identified?
Identifying achalasia early is crucial to prevent severe weight loss. Diagnosis typically involves:
1. Esophageal Manometry
The gold standard test. It measures the pressure and muscle coordination of the esophagus. Achalasia shows characteristic patterns of pressure abnormalities.
2. Barium Swallow X-ray
This imaging test reveals a dilated esophagus with a narrow LES (“bird’s beak” appearance).
3. Endoscopy
Direct visual examination to rule out other causes like cancer and assess the esophageal lining.
Doctors will also take a medical history focused on swallowing difficulties, regurgitation, and unintended weight loss — all important clues.
Lifestyle and Dietary Strategies for Managing Achalasia Weight Loss
While medical treatment is essential, patients can also improve intake and minimize weight loss with supportive strategies:
1. Food Texture Modification
Many people find it easier to eat softer foods that are easier to swallow, such as:
- Soups and broths.
- Mashed or pureed foods.
- Smooth, blended meals.
These reduce the effort needed to swallow and can help increase caloric intake gradually.
2. Smaller, Frequent Meals
Eating smaller portions more frequently can help the esophagus process smaller volumes at a time, reducing the discomfort of larger meals.
3. Hydration with Meals
Taking sips of water with meals can assist food passage.
4. Nutrient-Dense Foods
Nutritionists often recommend calorie-dense and high-protein foods (like yogurts, smoothies with proteins, and nutrient-rich shakes) to help patients meet calorie goals without large meal sizes.
5. Working With Professionals
Dietitians and speech-language pathologists can offer tailored advice to improve swallowing mechanics and nutritional outcomes.
When Weight Loss Signals a Need for Immediate Care
Sudden or rapid weight loss should always be taken seriously, especially if accompanied by:
- Increasing difficulty swallowing.
- Frequent regurgitation or vomiting.
- Severe chest pain.
- Signs of dehydration or weakness.
Unintentional weight loss is not normal and may indicate worsening achalasia or complications such as pseudoachalasia — a condition where cancer at the gastroesophageal junction mimics achalasia symptoms.
If someone suspects achalasia, they should seek medical evaluation without delay.
Summary: Can Achalasia Cause Weight Loss?
Yes — achalasia can cause weight loss, and it does so through a combination of factors:
- Difficulty swallowing leads to reduced food intake.
- Regurgitation prevents calories from reaching the stomach and being absorbed.
- Reduced caloric intake over time causes weight loss and can lead to malnutrition.
- Severity and subtype of achalasia influence how much weight loss a person may experience.
Weight loss is a common and clinically important symptom of achalasia and often improves with effective treatment. Recognizing the early signs of dysphagia and weight change is essential for timely diagnosis and preventing long-term complications.
Final Takeaway
Understanding the link between achalasia weight loss and swallowing dysfunction helps patients and caregivers recognize the condition sooner and take appropriate action. While weight loss can be distressing, modern diagnostic tools and treatments through effective treatment strategies and through herbal supplements designed for achalasia often make it possible to restore nutrition, improve quality of life, and prevent severe malnutrition.
If you or someone you know is struggling with persistent swallowing difficulties and unexplained weight loss, consult a healthcare professional — early intervention can make a significant difference.