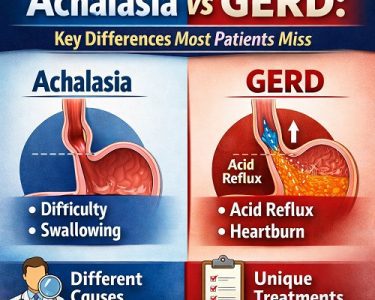
Achalasia is a rare, chronic disorder of the esophagus that affects swallowing and quality of life. It occurs when the nerve cells in the esophagus are damaged or destroyed, causing the lower esophageal sphincter (LES) – the muscle that normally relaxes to allow food into the stomach – to remain tight. As a result, food and liquids pool in the esophagus, leading to progressive dysphagia (difficulty swallowing), regurgitation, chest pain, cough, and weight loss. Because the underlying cause is largely unknown and the disease doesn’t resolve itself, finding the best treatment for achalasia is crucial for effective long-term symptom relief.
At present, no therapy cures achalasia or restores normal esophageal muscle function, but most treatments focus on opening the LES so that food can pass into the stomach more easily. This article comprehensively reviews the conventional treatment modalities — including surgery, balloon dilation, and the role (and limitations) of natural care, such as diet and lifestyle strategies — to help patients and caregivers understand their options and make informed choices.
Understanding Achalasia and Treatment Goals
Achalasia is characterized by:
- Failure of LES relaxation
- Absent peristalsis (no coordinated muscle contractions of the esophagus)
These features lead to a functional obstruction at the gastroesophageal junction, even though nothing physically blocks the path. Treatment aims to relieve this functional obstruction, improve esophageal emptying, and reduce symptoms such as dysphagia, chest pain, and regurgitation.
Because there is no cure, achieving symptom relief and improving quality of life are the ultimate goals. The best treatment for achalasia must balance effectiveness, long-term relief, safety, and patient preferences.
1. Surgical Treatments
Surgery is widely considered a highly effective long-term treatment option, especially for younger, otherwise healthy patients and those who need sustained relief. There are two main surgical approaches:
A. Heller Myotomy (Laparoscopic Heller Myotomy)
Heller myotomy is a surgical procedure in which the muscles of the LES are cut to lessen pressure and allow food to pass more easily into the stomach. Originally performed as an open surgery, it is now most often done via minimally invasive laparoscopy, which reduces pain, speeds recovery, and shortens hospital stays.
Because cutting the LES muscle increases the risk of gastroesophageal reflux disease (GERD), surgeons often perform a fundoplication at the same time — wrapping part of the stomach around the lower esophagus to reduce acid reflux.
Advantages:
- High long-term success rates: Many studies show excellent relief of symptoms after Heller myotomy, with success rates often over 85% to 90%.
- Durability: Problems such as dysphagia are less likely to recur compared to non-surgical treatments.
- Effective in most achalasia subtypes: Regardless of whether the LES problem is mild or severe, surgery reliably reduces the obstruction.
Disadvantages:
- Invasive: While laparoscopic, it still involves anesthesia and operative risks.
- Reflux risk: Even with fundoplication, some patients develop reflux afterward.
B. Peroral Endoscopic Myotomy (POEM)
Peroral endoscopic myotomy (POEM) is a newer, minimally invasive endoscopic surgery that achieves similar goals to a Heller myotomy but without external incisions. Surgeons create a tunnel inside the esophageal lining and cut the LES muscles from within.
Advantages:
- Minimal scarring: No external incisions.
- Shorter hospital stays and quicker recovery compared to traditional surgery.
- Highly effective: Many studies report success rates above 90%.
Disadvantages:
- Reflux risk: Some evidence suggests that acid reflux may be more common after POEM compared to Heller myotomy with fundoplication.
- Requires specialized skill: POEM is not as widely available and should be performed by experienced teams.
Comparing Surgical Options
Both laparoscopic Heller myotomy and POEM have demonstrated high efficacy in controlled studies, and neither is clearly superior in all cases. Choice often depends on:
- Patient age and overall health
- Achalasia subtype (diagnosed by manometry)
- Physician experience and local expertise
- Patient preferences and tolerance of reflux risk
Evidence suggests that both surgeries provide excellent long-term relief, and POEM is increasingly used as a first-line treatment in many centers because of its minimally invasive nature.
2. Balloon Dilation (Pneumatic Dilation)
Balloon dilation — sometimes called pneumatic dilation — is a key non-surgical option for people with achalasia. During the procedure, a balloon passed into the esophagus is inflated at the LES to stretch and partially tear the muscle fibers, reducing LES pressure and improving swallowing.
Advantages
- Less invasive: Performed endoscopically under sedation.
- Good symptom improvement: Many patients experience significant relief — studies have reported symptom improvement in up to 80-90% of patients.
- Outpatient: Short recovery compared to surgery.
Disadvantages
- Temporary and repetitive: Many patients need repeat dilations over time because LES tension tends to recur; around one-third of patients require repeat treatment within five years.
- Perforation risk: There is a small risk (about 1-2%) of esophageal perforation, which may require emergency surgery.
- Variable long-term durability: Some studies suggest slightly lower long-term relief compared with surgical myotomy.
Overall, balloon dilation remains an effective non-surgical strategy, particularly for patients who are older, have comorbid conditions that make surgery risky, or prefer a less invasive approach.
3. Medical and Other Non-surgical Therapies
In addition to pneumatic dilation, several non-surgical therapies may be considered:
A. Botulinum Toxin (Botox) Injection
Botox can be injected into the LES to relax muscles temporarily. The effect usually lasts 3–6 months and often needs repeating. Botox is most commonly used in patients who are not candidates for dilation or surgery (e.g., due to age or frailty).
B. Medications
Oral drugs such as nitrates and calcium channel blockers can decrease LES pressure slightly, but they generally provide only limited and short-lasting relief. These treatments are typically used temporarily or in patients who cannot undergo more definitive procedures.
C. Stents and Other Endoscopic Techniques
Some non-conventional treatments — such as temporary esophageal stents or sclerosing agents like polidocanol — have been explored, but evidence remains limited and they are not part of standard care.
D. Natural Remedies
Natural remedies also known as “Herbal Remedies”, one of the best non-surgical therapies. These remedies are made from the natural herbs and plant sources. If you want to buy it, visit our product page related to herbal remedies.
4. Natural Care and Lifestyle Approaches
Because achalasia is a mechanical problem (failure of LES relaxation due to nerve dysfunction), natural care alone cannot resolve the underlying condition. There is currently no scientific evidence that diet changes, supplements, or alternative therapies can replace surgery or dilation as definitive treatment.
However, lifestyle and diet modifications can help manage symptoms and support overall health, especially before treatment or while waiting for a procedure:
A. Nutrition and Diet Adjustments
Patients often adjust food consistency and eating habits to make swallowing easier and to maintain nutrition:
- Eating smaller, frequent meals
- Chewing thoroughly and eating slowly
- Choosing softer or pureed foods if needed
- Drinking warm liquids with meals, as some people find relief compared to cold foods
B. Positioning and Eating Habits
- Remaining upright after meals
- Eating earlier in the evening to reduce nighttime symptoms
- Some individuals find that sleeping in an elevated position (head of bed raised) can help with reflux symptoms
C. Professional Nutritional Support
Severe achalasia can lead to malnutrition and weight loss; dietitians can help tailor plans to meet nutrient needs and suggest supplements if necessary.
Comparing Treatments: What Does the Evidence Say?
When evaluating which approach offers the best treatment for achalasia, evidence supports the following key conclusions:
Effectiveness
- Surgical options (Heller myotomy and POEM) provide long-lasting symptom control and are generally considered more durable than balloon dilation alone for many patients.
- Balloon dilation offers a less invasive alternative with good initial success, but many patients will require repeat treatments.
- Botox and medications have more limited roles and are usually used when surgery and dilation are not appropriate.
Durability and Recurrence
- Surgery (especially Heller with fundoplication or POEM) often provides long-term relief with lower recurrence rates than repeated balloon dilations.
- Balloon dilation often needs to be repeated — and repeated procedures over time may become less effective.
Safety Profile
- Surgery carries operative risks but is generally safe in experienced hands.
- Balloon dilation has fewer immediate risks but carries a small risk of perforation.
Patient Selection Matters
- Age, overall health, subtype of achalasia, anatomy, and personal preferences all influence which treatment is most appropriate. Tailoring the choice to the individual yields the best outcomes.
Making the Choice: A Patient-Centered Approach
Choosing the best treatment for achalasia involves careful discussion between the patient and their gastroenterologist or surgeon. Considerations include:
1. Goals and Expectations
- Does the patient prioritize long-lasting relief or lower invasiveness?
- Are symptoms severe or mild?
- What are the lifestyle and work factors?
2. Medical Profile
- Age and overall health
- Ability to tolerate anesthesia or a procedure
- Risk factors for reflux or complications
3. Local Expertise
Not all medical centers offer advanced options like POEM; access to experienced surgeons and specialized care can shape the choice.
Conclusion
Achalasia is a chronic, progressive disorder for which no cure currently exists — but effective treatments are available. Among these:
- Surgery, particularly laparoscopic Heller myotomy and POEM, offers some of the most durable long-term relief and is often considered the best option for many patients.
- Balloon dilation provides a less invasive alternative, suitable for many patients, especially those who cannot undergo surgery.
- Natural care alone is not sufficient to treat achalasia, but diet and lifestyle adjustments play a supportive role in symptom management and nutrition.
Ultimately, the best treatment for achalasia depends on each patient’s unique situation — including symptom severity, health status, and personal preferences — and should be determined in consultation with experienced clinicians.