Achalasia is a rare but impactful esophageal motility disorder that makes swallowing progressively difficult and uncomfortable. While conventional medical approaches such as pneumatic dilation, medications, or surgical procedures are often effective, many individuals look for complementary options that support symptom relief, improve overall well-being, and potentially enhance esophageal function. This article explores natural treatment for achalasia, diving deep into the scientific basis, herbal remedies, lifestyle modifications, and evidence-based holistic strategies that may help improve swallowing and reduce symptom severity.
Understanding Achalasia: What Is It and How Does It Affect Swallowing?
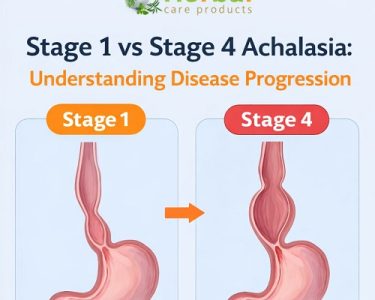
Achalasia is a chronic disorder of the esophagus characterized by two primary problems:
- Failure of the lower esophageal sphincter (LES) to relax properly
- Absence or reduction of normal esophageal peristalsis (muscular contractions)
In a healthy swallow, coordinated muscle contractions move food downward while the LES relaxes to allow food into the stomach. In achalasia, impaired nerve signaling prevents effective peristalsis, and the LES remains tight. The result: food and liquids back up in the esophagus, creating symptoms such as:
- Difficulty swallowing (dysphagia)
- Regurgitation
- Chest discomfort
- Heartburn
- Weight loss
- Coughing or aspiration
Because achalasia affects the neuromuscular coordination of the esophagus, patients often describe a feeling that food “gets stuck” after swallowing. Standard medical approaches focus on mechanically or chemically reducing LES pressure and managing symptoms. But a growing number of individuals seek a natural treatment for achalasia to supplement other therapies.
Why People Consider Natural Treatments
Patients pursue natural or alternative therapies for several reasons:
- Desire to minimize medication side effects
- Preference for holistic care
- Strong interest in lifestyle approaches
- Desire for supportive therapies between medical interventions
It’s important to be clear: natural treatments should never replace medically indicated therapy for achalasia—particularly in moderate to severe cases. Instead, herbs and lifestyle support may help ease symptoms, improve quality of life, and work alongside conventional care.
Can Herbs Help Improve Swallowing? The Evidence
Herbal remedies have been used for digestive issues for centuries. However, when it comes to achalasia specifically, clinical research is limited. Most available studies focus on broader gastrointestinal motility, inflammation, and esophageal comfort. So while the evidence is not definitive, several herbs show promise based on their effects on:
- Smooth muscle function
- Spasm relief
- Inflammation reduction
- Nervous system soothing
Below are some herbs commonly discussed in the context of digestive support and potential symptom relief.
Herbs That May Support Swallowing and Esophageal Comfort
1. Licorice Root (Glycyrrhiza glabra)
Properties:
- Soothing demulcent (forms a protective lining)
- Anti-inflammatory
- Mild antispasmodic
Licorice root has a long history in digestive health, especially for soothing mucosal irritation. As a demulcent, licorice may help form a protective layer over irritated esophageal tissue. Some derivatives like deglycyrrhizinated licorice (DGL) are often recommended to avoid side effects associated with whole licorice, such as high blood pressure.
How it might help:
By coating irritated tissues and reducing inflammation, licorice may lessen burning, discomfort, and irritation from stasis of food in the esophagus.
Caution:
Whole licorice should be used with care due to potential effects on blood pressure and potassium balance. Deglycyrrhizinated forms are generally safer for long-term use.
2. Ginger (Zingiber officinale)
Properties:
- Digestive aid
- Anti-nausea
- Mild smooth muscle relaxant
Ginger is well known as a digestive aid that supports motility and can reduce nausea. While it does not directly increase esophageal peristalsis, its ability to support overall gut movement and reduce discomfort may be helpful for individuals with achalasia.
How it might help:
By easing gastric discomfort and promoting motility lower in the digestive tract, ginger could indirectly support more comfortable swallowing and downstream digestion.
Best use:
Fresh ginger tea, tinctures, or standardized extracts taken before or after meals.
3. Chamomile (Matricaria chamomilla)
Properties:
- Calming antispasmodic
- Anti-inflammatory
- Nervine (soothes nervous tension)
Chamomile’s gentle antispasmodic and calming effects may help reduce esophageal muscle spasms and stress-induced tightening during swallowing.
How it might help:
By reducing muscle tension and inflammation, chamomile may provide comfort and reduce the sensation of tightness.
Best use:
Chamomile tea after meals or during moments of stress associated with eating.
4. Slippery Elm (Ulmus rubra)
Properties:
- Mucilage-rich (soothing and protective)
- Demulcent
Like licorice, slippery elm contains mucilage, which can coat and soothe irritated membranes. It has been used traditionally to ease sore throats and digestive irritation.
How it might help:
The mucilage may help protect the esophageal lining and ease the passage of food that lingers in the lower esophagus.
Best use:
Slippery elm bark powder mixed with warm water after meals.
5. Marshmallow Root (Althaea officinalis)
Properties:
- Soothing demulcent
- Anti-inflammatory
Marshmallow root also contains high levels of mucilage, which can create a protective coating along mucous membranes.
How it might help:
Coating the esophagus may provide symptomatic relief from irritation caused by food back-up and regurgitation.
Best use:
Marshmallow root tea or infusion, taken gently after meals.
6. Peppermint (Mentha piperita) – With Caution
Peppermint is often touted for digestive comfort and antispasmodic activity. However, in individuals with reflux or weak LES function, peppermint can relax the sphincter further, potentially worsening symptoms.
Best practice:
Use peppermint cautiously and consider personal tolerance.
Important Note on Herbal Use
While herbs can offer comfort and support digestion, the esophageal dysfunction in achalasia is structural and neurologic in nature. That means herbs are generally aimed at symptom support rather than correcting the underlying motility problem. Always consult a healthcare provider before starting herbal remedies—especially if taking other medications or having underlying health conditions.
Other Natural Treatment Approaches for Achalasia
Beyond herbs, several lifestyle and non-pharmacologic achalasia treatment strategies may improve symptoms and support easier swallowing.
1. Dietary Adjustments
Diet plays a central role in achalasia management. Because swallowed food moves slowly, small changes can significantly affect comfort.
Swallowing-Friendly Approaches
- Eat smaller, frequent meals: Reduces pressure on the esophagus and LES.
- Choose softer foods: Purees, smoothies, soups, well-cooked vegetables, mashed potatoes, yogurts, eggs, and tender proteins.
- Avoid dry/sticky foods: Bread, crackers, rice cakes—these can lodge in the esophagus more easily.
- Stay upright while eating and for at least 30 minutes after meals
- Drink water or tea with food: Helps wash food downward.
Patients often find that modifying food texture dramatically reduces the sensation of “stuck food.”
2. Hydration Habits
Adequate hydration is essential for everyone but especially for people with achalasia. Sipping water throughout meals can help propel food through the esophagus.
Some people benefit from:
- Warm water with meals
- Carbonated water (sparingly, as carbonation can worsen bloating)
Hydration also supports overall digestion and may reduce irritation from slow clearance.
3. Gentle Physical Practices
Some mind-body practices have been explored for supporting digestive comfort and reducing muscular tension:
Yoga and Breathing Techniques
- Diaphragmatic breathing
- Gentle twists
- Post-meal restorative poses
These practices may help relax the diaphragm and reduce stress-related tension, which can impact swallowing comfort.
Gentle Walking After Meals
Light movement may support downstream motility and enhance comfort.
4. Heat Therapy
Applying warm compresses or heat packs to the chest area can:
- Reduce muscular tension
- Promote blood flow
- Provide comfort during flare-ups
Heat should be gentle and comfortable, not hot enough to cause burns.
5. Acupuncture and Traditional Therapies
Some individuals explore acupuncture and related traditional modalities for digestive motility and nervous system regulation.
While scientific evidence remains limited, acupuncture may:
- Reduce stress
- Calm the nervous system
- Help with gastrointestinal discomfort
Persons considering acupuncture should work with licensed practitioners familiar with gastrointestinal conditions.
6. Natural Supplements
Some people go with natural supplements, because they provide relief naturally. These natural supplements are made from natural sources like herbs and plant extracts.
Stress, Anxiety, and Swallowing
Swallowing difficulty inherently raises anxiety. Anxiety can paradoxically exacerbate the sensation of food getting stuck. Breaking this cycle can be an essential part of natural treatment for achalasia.
Recommended Strategies
- Mindful eating (slow, intentional, without distraction)
- Meditation before meals
- Progressive muscle relaxation
- Support groups or counseling
By reducing overall tension, patients may find swallowing becomes easier over time.
Supplements That Have Been Discussed (With Caution)
A few supplements are often mentioned in digestive support discussions:
Probiotics
Probiotics may help maintain gut microbiome balance, but they don’t directly improve esophageal motility. However, they may reduce associated symptoms like bloating or gas.
Digestive Enzymes
May help with breakdown of food after swallowing but do not affect the LES or peristalsis directly.
Magnesium
Magnesium may reduce muscle tension. Some individuals report improved smooth muscle relaxation with magnesium supplementation. Always consult a physician before use.
What Natural Approaches Cannot Replace
While herbs and lifestyle modifications can ease symptoms and improve comfort, they cannot correct the fundamental motility disorder underlying achalasia. Therefore, it is important to understand when medical intervention is required.
Consider medical assessment if:
- Swallowing difficulty worsens
- Weight loss occurs
- Repeated regurgitation or aspiration
- Chest pain increases
- Difficulty managing nutrition
Standard medical approaches include:
- LES-targeted medications (e.g., calcium channel blockers)
- Botulinum toxin injections
- Pneumatic dilation
- Heller myotomy
- Peroral endoscopic myotomy (POEM)
These options are typically managed by a gastroenterologist and, when appropriate, a surgeon.
Combining Approaches: A Holistic Strategy
For many individuals, the most effective strategy blends conventional medical care with supported natural treatments. This may include:
- Medical management of LES pressure
- Dietary texture modifications
- Herbal support for irritation and comfort
- Hydration and mindful eating
- Stress-reduction techniques
- Physical movement and gentle exercise
This multimodal approach acknowledges that while herbs and lifestyle changes may not cure achalasia, they can play a valuable role in overall comfort and quality of life.
Case Examples
Case Example 1: Gentle Relief Through Diet and Herbs
Sarah, a 42-year-old woman with mild achalasia, struggled with frequent sensations of food sticking. After working with her physician, she adopted:
- Soft diet with blended soups and smoothies
- Slippery elm tea after meals
- Warm water with each bite
- Gentle yoga breathing
She reported reduced discomfort and fewer episodes of food sticking. While her core motility issues remained, symptom severity decreased.
Case Example 2: Managing Anxiety and Eating Habits
Mark, a 58-year-old man, found that anxiety around eating worsened his symptoms. By practicing:
- Mindfulness before meals
- Chamomile tea to relax before eating
- Slow deliberate chewing habits
Mark noticed that anxiety no longer triggered his worst symptoms, and his overall quality of life improved.
Safety and Precautions
When exploring natural treatment for achalasia:
- Never stop prescribed medical treatments without a physician’s approval.
- Discuss herbal remedies with your doctor, especially if taking other medications.
- Be cautious of herb–drug interactions, particularly with blood pressure or anticoagulant medications.
- Recognize that not all herbs suit all individuals—personal sensitivity matters.
- Avoid self-treating moderate/severe achalasia without medical supervision.
Frequently Asked Questions (FAQs)
1. Can natural remedies cure achalasia?
No. Natural remedies may help ease symptoms and improve comfort, but they cannot cure achalasia’s underlying neuromuscular dysfunction.
2. Are herbs safe for everyone with achalasia?
Not always. Individuals with heart conditions, high blood pressure, or on multiple medications should consult a healthcare provider before trying herbs.
3. Can diet alone fix swallowing difficulties?
Diet alone rarely resolves achalasia but can significantly improve daily comfort and reduce symptom burden.
4. How quickly might herbs show results?
Some individuals notice soothing effects within days, while others may take weeks. Herbs often support comfort rather than directly changing disease mechanisms.
Conclusion: Balancing Nature and Medicine
Achalasia is a complex condition rooted in disrupted esophageal motility. While conventional medical treatments are the foundation of effective management, natural treatment for achalasia using herbs and lifestyle practices can offer supportive relief, enhance comfort, and improve quality of life.
Herbs like licorice (DGL), slippery elm, marshmallow root, ginger, and chamomile may help by soothing irritation, reducing inflammation, and calming muscle tension. Dietary modifications, hydration, gentle physical activity, and stress management further support well-being. These all strategies are important for achalasia daily management. However, these approaches should be viewed as complementary—not substitutive—to medical care under the guidance of healthcare professionals.
By blending evidence-based natural strategies with conventional medicine, individuals can create a balanced, holistic plan to improve swallowing comfort and overall digestive health.