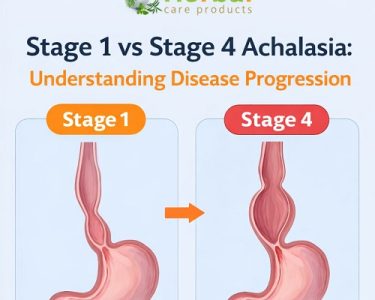
Achalasia is a rare but significant disorder of the esophagus—a tube that carries food from your mouth to your stomach. When achalasia occurs, the lower esophageal sphincter (LES)—a muscular valve at the bottom of the esophagus—fails to relax properly. This makes swallowing difficult and can lead to symptoms such as regurgitation, chest pain, heartburn, and weight loss.
One of the most effective long-term treatments for achalasia is Heller myotomy, a surgical procedure that cuts the tight LES muscle to ease swallowing. But while the procedure itself is a critical step, many people wonder: what happens after surgery? What does achalasia surgery recovery involve? What challenges might you face, and how long before you can eat normally again or return to your daily routine?
In this article, we’ll walk you through everything you need to know about achalasia surgery recovery—from the first hours after your operation all the way through months of healing and long-term life after Heller myotomy.
Understanding Heller Myotomy: A Quick Primer
Before diving into recovery, it helps to understand what a Heller myotomy actually does:
- It’s a surgical technique that cuts the muscle fibers of the LES so that food can pass into the stomach more easily. Most Heller myotomies today are done laparoscopically, meaning through small incisions with a camera and instruments, which speeds recovery and reduces pain compared with traditional open surgery.
- Because the LES is loosened during the procedure, many surgeons perform a fundoplication at the same time—wrapping part of the stomach around the esophagus—to help prevent reflux afterward.
It’s important to note that Heller myotomy does not cure achalasia, but it can dramatically improve symptoms and quality of life for many people.
What to Expect Immediately After Surgery
In the Recovery Room (Hours After Surgery)
Once your surgery is completed, you will be moved to a recovery area:
- You’ll wake up from anesthesia in a monitored setting.
- Nurses will check your vital signs (heart rate, blood pressure, oxygen levels, etc.).
- Pain and nausea are common at first, and medications will be provided to keep you comfortable.
Many patients report mild to moderate discomfort around the incision sites as the anesthesia wears off, but this typically diminishes quickly, especially with minimally invasive (laparoscopic) surgery.
Hospital Stay (1–3 Days)
Most people stay in the hospital for one to three days after Heller myotomy. Here’s what typically happens during this phase:
- Day 1: Clear liquids are introduced as tolerated (broth, water, tea, Jell-O).
- Day 2: You may begin fuller liquids or very soft foods, depending on your surgeon’s guidance.
- Doctors may do imaging—such as a barium swallow—to ensure there’s no leak or complication before progressing your diet.
Your team will also review pain management, activity recommendations, and signs to watch for that could suggest a complication.
Achalasia Surgery Recovery Timeline
Recovery isn’t instant. Healing happens over time, and understanding the phases can help you set realistic expectations.
First Week After Surgery
This phase is all about healing and rest.
- Pain and Discomfort: Most people feel soreness around the incision sites and some chest discomfort. Pain meds and rest help manage this.
- Eating and Diet: You may remain on liquids or soft foods. Clear liquids usually progress to more nutrient-rich options like strained soups, yogurt, and smoothies.
- Activity: Short walks are encouraged to prevent blood clots and help digestion, but avoid strenuous exertion or heavy lifting.
Even if symptoms improve quickly, take your time—swelling in the esophagus and incision sites needs time to settle.
2–4 Weeks After Surgery
By this point, you should notice steady improvement:
- Diet Progression: Many people can start soft foods around this time and slowly reintroduce more solid foods. Chewing thoroughly and eating smaller meals helps.
- Return to Work: Light, non-physically demanding work may be possible during this period for many people.
- Symptoms: Many notice a significant reduction in dysphagia (difficulty swallowing) and less regurgitation.
However, everyone heals at their own pace, and some people may still feel tired or uncomfortable during this phase.
6–8 Weeks After Surgery
This is a major milestone in achalasia surgery recovery:
- Normal Activities: Most daily activities, including driving, grocery shopping, and mild exercise, are usually fine by now.
- Lifting and Strenuous Exercise: Heavy lifting and intense workouts are often restricted until your surgeon gives the go-ahead.
- Diet: Many people can enjoy most foods, though some may need to continue being cautious with tough, dry, or very acidic items.
3 Months and Beyond
At three months, many people feel substantially recovered:
- Swallowing Function: Dysphagia continues to improve as swelling subsides and your esophagus adjusts.
- Lifestyle: Normal living—with appropriate diet choices—becomes more manageable, and many people return to almost pre-surgery life.
- Long-Term Follow-Up: Regular check-ups help detect issues like reflux or recurring symptoms. Annual or periodic upper GI evaluations may be recommended.
Note that in some individuals, complete esophageal healing can take many months—up to six or even eight months.
Important Considerations During Recovery
Pain and Discomfort
It’s normal to have soreness and discomfort after surgery. Typical sources include:
- Incision pain
- Mild chest or shoulder discomfort (from gas used during laparoscopy)
- Muscle soreness from coughing or movement
Pain usually improves significantly after the first several days, but each person’s pain threshold and healing capacity vary.
Diet and Swallowing
Dietary progression is a cornerstone of achalasia surgery recovery:
- Clear liquids → 2. Full liquids → 3. Soft foods → 4. Gradual return to solids
This slow advancement helps your body adapt and prevents strain or discomfort.
Chew thoroughly and eat smaller meals. Staying upright while eating and for at least half an hour afterward helps food move smoothly.
Activity and Exercise
- Light activity—like short walks—promotes circulation and healing.
- Avoid heavy lifting and intense workouts until your surgeon approves.
Some people find it helpful to keep an activity journal to track how they feel with each progression.
Reflux and Heartburn
Because the LES is loosened during Heller myotomy, gastroesophageal reflux disease (GERD) can become more common after surgery. That’s why many surgeons perform a fundoplication at the same time:
- Fundoplication creates a flap to help reduce reflux.
- Some people may still need blood-acid reducing medications temporarily (and occasionally long-term).
Be alert for persistent heartburn, especially at night or when lying flat.
Potential Challenges and When to Seek Help
Achalasia surgery recovery is usually smooth, but complications can occur. Contact your healthcare provider if you experience:
- Fever, chills, or signs of infection
- Increasing pain that doesn’t respond to medication
- Inability to swallow even liquids
- Chest pain that feels sharp or radiates
- New-onset or worsening shortness of breath
- Persistent vomiting or inability to keep fluids down
Long-Term Outlook: Life After Recovery
For many people, achalasia surgery offers significant and lasting relief from symptoms. Studies show that:
- A high percentage of patients enjoy long-term symptom improvement after Heller myotomy.
- Some people may require additional interventions years later if symptoms recur, but most enjoy years of better swallowing and fewer regurgitation issues.
Remember: postoperative follow-up is critical. Achalasia is chronic, and lifelong monitoring helps ensure that changes—like reflux or recurrent symptoms—are detected and managed early.
Real Patient Perspectives on Recovery
Real experiences (from online patient discussions) echo many of the general timelines mentioned above:
- Some people feel significantly better within a few weeks but caution that the healing process continues over months.
- Others stress patience—especially with food progression and energy levels.
- Multiple stories highlight that many return to activities and even travel within a few months, provided they follow their doctor’s guidance.
These real-world perspectives reinforce that recovery is gradual, and each person’s timeline may vary.
Conclusion: Achalasia Surgery Recovery—A Journey Worth Taking
Recovering from achalasia surgery like Heller myotomy is a step-by-step journey, not a single moment. It involves:
- A careful diet progression
- Gradual increase in activity
- Mindful attention to symptoms
- Ongoing medical follow-up
Understanding what to expect—from the first post-op days in the hospital to months of healing before feeling fully yourself—can reduce anxiety and help you recover with confidence.
If you have upcoming surgery or are currently navigating recovery, keep in close contact with your healthcare team. With patience, proper care, and realistic expectations, achalasia surgery recovery can lead to significant and lasting improvements in swallowing and quality of life.
Explore our Product Page: “Home Remedies for Achalasia”