Achalasia is a rare but serious disorder of the esophagus that affects a person’s ability to swallow food and liquids properly. Although uncommon, Achalasia can significantly impact quality of life when left untreated. Many people initially mistake its symptoms for acid reflux or heartburn, which often delays proper diagnosis.
Achalasia—including its causes, symptoms, diagnostic procedures, conventional treatments, dietary recommendations, natural support options and how it differs from GERD bescause achalasia is dangerous if untreated.
What is Achalasia?
Achalasia is a chronic motility disorder of the esophagus—the muscular tube that carries food from the mouth to the stomach. In people with Achalasia, two main problems occur:
- The lower esophageal sphincter (LES)—the muscle valve between the esophagus and stomach—fails to relax properly.
- The esophageal muscles lose their normal wave-like contractions (peristalsis) that move food downward.
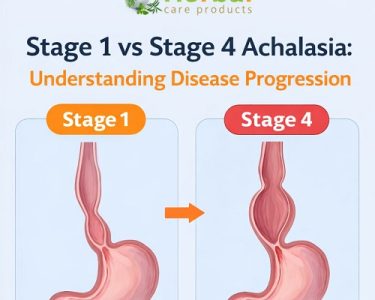
As a result, food and liquids accumulate in the esophagus instead of entering the stomach. Over time, the esophagus may become enlarged, stretched, and less functional.
Achalasia affects men and women equally and typically appears between ages 25 and 60, though it can occur at any age. It is considered rare, affecting approximately 1 in 100,000 people per year.
Causes of Achalasia
The exact cause of Achalasia is not fully understood, but research suggests it involves damage to the nerves that control esophageal muscles.
1. Nerve Degeneration
The most widely accepted theory is degeneration of nerve cells (ganglion cells) in the esophageal wall. These nerves normally coordinate muscle relaxation and contraction. When they are damaged, the LES remains tightly closed and peristalsis weakens or stops.
2. Autoimmune Factors
Some researchers believe Achalasia may be an autoimmune condition, where the body’s immune system mistakenly attacks the esophageal nerves.
3. Viral Infections
Certain viral infections have been proposed as triggers for immune-mediated nerve damage, although clear evidence is still lacking.
4. Genetic Factors
While Achalasia is generally not inherited, rare familial cases suggest a possible genetic predisposition in some individuals.
5. Secondary Achalasia (Pseudoachalasia)
In rare instances, Achalasia-like symptoms may result from other conditions, including cancers near the gastroesophageal junction. Proper diagnostic evaluation is critical to rule out these causes.
Achalasia Symptoms
The symptoms of Achalasia often develop gradually and worsen over time. Early signs may be subtle and easily confused with acid reflux.
1. Difficulty Swallowing (Dysphagia)
This is the hallmark symptom of Achalasia. People typically have trouble swallowing both solids and liquids—unlike other conditions where solids are more problematic. If you want to explore more about this, you can read our another article in which Achalasia and Difficulty Swallowing Explained in details.
2. Regurgitation
Undigested food may come back up into the mouth, especially when lying down. This can lead to coughing or choking during sleep.
3. Chest Pain
Some individuals experience chest discomfort or pressure, sometimes mistaken for heart-related pain.
4. Weight Loss
Difficulty eating often leads to unintentional weight loss and malnutrition.
5. Heartburn-like Symptoms
Although Achalasia is not acid reflux, food retention can cause irritation and a burning sensation.
6. Chronic Cough or Aspiration
Food or liquid entering the airways can cause coughing, pneumonia, or respiratory infections.
If these symptoms persist, medical evaluation is essential. Delayed treatment may lead to complications such as esophageal dilation or increased risk of esophageal cancer.
How Achalasia Is Diagnosed
Because Achalasia symptoms overlap with other digestive disorders, accurate diagnosis requires specialized testing that’s why a question raised by many people question how achalasia is diagnosed, let’s explore it.
1. Esophageal Manometry (Gold Standard)
High-resolution esophageal manometry measures muscle contractions and LES relaxation. This is the most definitive test for Achalasia and classifies it into subtypes (Type I, II, III), which guide treatment decisions.
2. Barium Swallow (Esophagram)
In this imaging test, the patient swallows a barium solution that coats the esophagus. X-rays reveal a classic “bird’s beak” narrowing at the LES.
3. Upper Endoscopy (EGD)
An endoscope is inserted through the mouth to examine the esophagus and stomach. This helps rule out cancer or structural causes.
Early diagnosis significantly improves treatment outcomes and reduces complications.
Conventional Treatment Options
There is currently no cure for Achalasia, but several effective best treatments for achalasia relieve symptoms by relaxing or weakening the LES.
1. Pneumatic Dilation
A balloon is inserted endoscopically and inflated to stretch and partially tear the LES muscle. This improves swallowing but may require repeat procedures.
2. Heller Myotomy
A surgical procedure in which the LES muscle is cut to allow easier passage of food. It is often combined with partial fundoplication to reduce reflux.
3. Peroral Endoscopic Myotomy (POEM)
A minimally invasive endoscopic technique that cuts the LES from within the esophagus. POEM has become increasingly popular due to its high success rates.
4. Botulinum Toxin (Botox) Injections
Botox relaxes the LES temporarily. This option is generally reserved for older adults or those who cannot undergo surgery.
5. Medications
Calcium channel blockers or nitrates may reduce LES pressure, but they are typically less effective and used when other treatments are not suitable.
Each treatment has risks and benefits. A gastroenterologist helps determine the best approach based on patient age, health status, and Achalasia subtype.
Best Foods to Include in a Diet Plan for Achalasia
Best foods to include in a diet plan for achalasia are given below:
1. Soft Proteins
Protein is essential to prevent muscle loss and weight loss.
Good options:
- Scrambled eggs
- Soft tofu
- Well-cooked fish
- Shredded chicken with gravy
- Lentil soup
- Greek yogurt
Avoid dry meats or large chunks.
2. Smooth Carbohydrates
Carbohydrates provide needed energy.
Best choices:
- Mashed potatoes
- Oatmeal
- Cream of wheat
- Soft rice or rice porridge
- Well-cooked pasta with sauce
Avoid crusty bread and dry crackers.
3. Cooked Fruits and Vegetables
Raw produce may be difficult to swallow.
Better options:
- Steamed carrots
- Pumpkin puree
- Applesauce
- Ripe bananas
- Avocado
- Blended vegetable soups
Avoid raw salads or fibrous vegetables like celery.
4. Healthy Fats for Extra Calories
Maintaining weight can be difficult. Add:
- Olive oil
- Nut butters (smooth)
- Avocado
- Full-fat dairy
- Smoothies with protein powder
Fats make meals softer and easier to swallow.
Foods to Avoid in a Diet Plan for Achalasia
Certain foods commonly worsen symptoms:
❌ Dry Foods
- Toast
- Crackers
- Dry rice
- Overcooked meat
❌ Tough or Fibrous Foods
- Steak
- Raw cabbage
- Celery
- Pineapple
❌ Sticky Foods
- Peanut butter (thick)
- Chewy bread
- Dried fruits
❌ Carbonated Drinks
They increase pressure and bloating.
Sample 7-Day Diet Plan for Achalasia
Here is a practical weekly plan.
Day 1
Breakfast: Oatmeal with mashed banana
Snack: Yogurt
Lunch: Lentil soup + soft rice
Snack: Smoothie
Dinner: Baked fish + mashed potatoes
Day 2
Breakfast: Scrambled eggs
Snack: Applesauce
Lunch: Chicken broth with soft noodles
Snack: Avocado toast (soft bread)
Dinner: Steamed vegetables + tofu
Day 3
Breakfast: Cream of wheat
Snack: Protein shake
Lunch: Vegetable puree soup
Snack: Cottage cheese
Dinner: Soft pasta with white sauce
Day 4
Breakfast: Smoothie with oats
Snack: Ripe banana
Lunch: Soft khichdi (rice and lentils)
Snack: Yogurt
Dinner: Shredded chicken with gravy
Day 5
Breakfast: Soft pancakes with syrup
Snack: Fruit puree
Lunch: Mashed potatoes + soft fish
Snack: Protein smoothie
Dinner: Pumpkin soup
Day 6
Breakfast: Scrambled eggs
Snack: Applesauce
Lunch: Soft rice + dal
Snack: Avocado smoothie
Dinner: Pasta with soft vegetables
Day 7
Breakfast: Oatmeal
Snack: Yogurt
Lunch: Chicken soup
Snack: Cottage cheese
Dinner: Soft vegetable stew
Natural Remedies for Achalasia
Medical treatments such as pneumatic dilation, Botox injections, or surgical procedures like Heller myotomy are often effective. However, many patients:
- Want to reduce symptom severity naturally
- Seek complementary support after procedures
- Prefer non-invasive symptom management
- Experience mild or early-stage achalasia
Natural remedies for achalasia do not replace medical treatment but can significantly improve comfort and digestive function.
1. Dietary Modifications: The Foundation of Natural Management
One of the most effective Natural Remedies for Achalasia is adjusting your diet.
Eat Soft, Easy-to-Swallow Foods
Soft foods reduce pressure on the esophagus. Examples include:
- Mashed vegetables
- Yogurt
- Smoothies
- Oatmeal
- Scrambled eggs
- Soups and broths
Avoid Dry or Tough Foods
Steak, dry bread, raw vegetables, and tough meats may worsen swallowing difficulty.
Take Smaller, Frequent Meals
Large meals increase esophageal pressure. Eating smaller portions 5–6 times daily may reduce symptoms.
Chew Thoroughly and Eat Slowly
Proper chewing makes food easier to pass through the LES.
2. Stay Hydrated During Meals
Drinking warm water while eating can help food move through the esophagus more smoothly.
Why Warm Liquids Help
Warm fluids may relax esophageal muscles slightly and assist food passage.
Best options:
- Warm water
- Herbal teas
- Light broths
Avoid:
- Very cold drinks
- Carbonated beverages
3. Elevate Your Head While Sleeping
Regurgitation at night is common in achalasia. Elevating the head 6–8 inches can prevent food from flowing back up.
You can:
- Use a wedge pillow
- Adjust your bed frame
- Place blocks under the bed legs
This simple method is one of the most practical Natural Remedies for Achalasia.
4. Herbal Remedies That May Help
Certain herbs may support digestion and reduce discomfort.
Ginger
Known for digestive support, ginger may:
- Reduce nausea
- Improve digestive motility
- Soothe inflammation
Drink ginger tea after meals.
Chamomile
Chamomile tea may:
- Relax smooth muscles
- Reduce inflammation
- Promote better sleep
Slippery Elm
This herb forms a soothing coating along the esophagus, potentially reducing irritation.
⚠ Always consult a healthcare provider before starting herbal supplements.
5. Stress Reduction and Relaxation Techniques
Stress can worsen digestive symptoms. Although achalasia is not caused by stress, tension may intensify discomfort.
Helpful Techniques:
- Deep breathing exercises
- Yoga
- Meditation
- Gentle stretching
- Progressive muscle relaxation
Mind-body therapies are valuable Natural Remedies for Achalasia because they promote overall digestive relaxation.
6. Esophageal-Friendly Eating Techniques
Changing how you eat can be just as important as what you eat.
- Sit upright while eating
- Remain upright for 2–3 hours after meals
- Take small bites
- Alternate food with sips of warm liquid
Gravity plays a key role in helping food move toward the stomach.
7. Maintain a Healthy Weight
Excess weight can increase abdominal pressure and worsen regurgitation. Maintaining a healthy body weight may:
- Reduce reflux-like symptoms
- Improve breathing
- Decrease nighttime discomfort
However, unintended weight loss is common in achalasia. Work with a healthcare provider to ensure adequate nutrition.
8. Gentle Physical Activity
Light exercise supports digestive health.
Recommended activities:
- Walking after meals
- Gentle yoga
- Stretching
Avoid heavy lifting or intense exercise immediately after eating.
9. Avoid Trigger Foods
Some foods may worsen symptoms:
- Spicy foods
- Fried or fatty meals
- Alcohol
- Caffeine
- Citrus fruits (if irritating)
Keeping a food journal can help identify personal triggers.
10. Nutritional Support
Because swallowing difficulty can reduce calorie intake, focus on nutrient-dense foods:
- Protein smoothies
- Nut butters
- Avocado
- Soft legumes
- Blended soups with added protein
Consider consulting a registered dietitian for personalized guidance.
11. Breathing Exercises for Esophageal Relaxation
Diaphragmatic breathing may reduce chest tightness.
How to Practice:
- Sit upright
- Inhale slowly through the nose
- Expand the abdomen
- Exhale slowly through the mouth
Practice for 5–10 minutes daily.
12. Probiotics for Digestive Balance
While achalasia primarily affects the esophagus, gut health still matters. Probiotics may:
- Improve overall digestion
- Reduce bloating
- Support immune function
Choose high-quality probiotic strains and consult your doctor before starting supplements.
13. Acupuncture and Complementary Therapies
Some individuals report symptom relief with acupuncture. Though evidence is limited, it may:
- Support nerve regulation
- Improve relaxation
- Reduce chest discomfort
Complementary approaches should be used alongside medical supervision.
Achalasia vs GERD
Achalasia and GERD (Gastroesophageal Reflux Disease) share some overlapping symptoms but are fundamentally different conditions.
Key Differences
| Feature | Achalasia | GERD |
| Cause | Nerve damage affecting LES relaxation | Weak LES allowing acid reflux |
| Swallowing | Difficulty with solids and liquids | Usually solids first |
| Acid Reflux | Not primary issue | Primary symptom |
| Treatment | LES muscle disruption | Acid suppression (PPIs) |
GERD is caused by a weak LES, while Achalasia involves a LES that fails to relax. Misdiagnosis is common, so specialized testing is important.
Living With Achalasia
Achalasia is a chronic condition, but with appropriate treatment, most people lead normal, active lives.
Long-Term Monitoring
Patients may require periodic evaluations to:
- Monitor esophageal dilation
- Assess swallowing function
- Screen for rare complications such as esophageal cancer
Emotional and Psychological Impact
Chronic swallowing difficulty can cause anxiety around eating. Support groups and counseling may be helpful.
Practical Tips
- Sleep with the head elevated.
- Keep water nearby during meals.
- Plan meals carefully when traveling.
- Maintain regular follow-up with a gastroenterologist.
Outlook
With modern treatments such as POEM and laparoscopic surgery, symptom control rates exceed 80–90%. Early intervention significantly improves outcomes.
Conclusion
Achalasia is a rare but impactful esophageal disorder characterized by impaired swallowing due to nerve dysfunction. Although its exact cause remains unclear, early recognition and proper diagnosis are essential to prevent complications.
Treatment options—including pneumatic dilation, surgical myotomy, and POEM—offer highly effective symptom relief. While natural remedies or natural treatment for achalasia and dietary adjustments and daily management for achalasia are also very effective for this disease, they can support overall digestive comfort and quality of life.
If you experience persistent difficulty swallowing both solids and liquids, unexplained regurgitation, or chest discomfort, consult a healthcare professional for evaluation. Early diagnosis and tailored treatment can dramatically improve long-term outcomes.
Understanding Achalasia empowers patients to seek timely care, make informed decisions, and live well despite this chronic condition. Achalasia occurs in different stages, if you want to explore it, you can read our blog in which Achalasia stages explained.