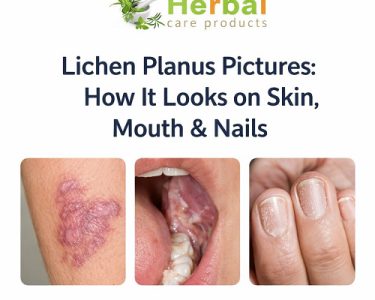
Lichen Planus is a chronic inflammatory condition that affects the skin and mucous membranes. Many people who notice unusual rashes or persistent irritation often ask, “What is Lichen Planus?” In simple terms, it is a disorder in which the immune system mistakenly attacks healthy skin or mucosal cells, leading to inflammation and distinctive lesions. The condition typically appears as purple, flat-topped, itchy bumps on the skin, but it can also affect other parts of the body. Although Lichen Planus is not contagious, it can cause significant discomfort and may persist for weeks, months, or even years in some cases.
This condition is considered important in dermatology and general health because it does not only affect the outer skin. Lichen Planus can involve multiple areas of the body, including the skin, mouth, scalp, nails, and genitals. For example, oral lichen planus may appear as white, lacy patches or painful sores inside the mouth, while scalp involvement can lead to redness, irritation, and even hair loss in severe cases. Because of its wide range of symptoms and affected areas, early recognition and proper management are essential.
Lichen Planus can occur in people of all ages, but it is most commonly seen in middle-aged adults, particularly those between the ages of 30 and 60. Both men and women can develop the condition, although certain forms, such as oral lichen planus, are more frequently observed in women. While the exact cause is not fully understood, researchers believe that immune system abnormalities, genetic factors, infections, medications, and stress may contribute to its development.
The symptoms of Lichen Planus vary depending on the area affected but often include itchy rashes, discoloration, sores, and changes in nails or hair. Diagnosis usually involves a physical examination and sometimes laboratory tests or a skin biopsy. Fortunately, various Lichen Planus treatment options are available, including topical medications, oral drugs, and lifestyle adjustments to reduce symptoms and inflammation.
Although it cannot always be completely prevented, understanding Lichen Planus causes, recognizing early signs, and seeking timely medical advice can help manage the condition effectively and reduce complications.
What is Lichen Planus?
Lichen Planus is a chronic inflammatory condition that affects the skin and mucous membranes. It is characterized by the appearance of itchy, flat-topped, purplish bumps on the skin or white, lace-like patches inside the mouth and other mucosal surfaces. When people ask “What is Lichen Planus?”, it can be described as a disorder in which the body’s immune system mistakenly attacks its own skin or mucous membrane cells, causing inflammation, irritation, and visible lesions. Although the condition can be uncomfortable and sometimes persistent, it is not contagious and cannot spread from person to person.
Medically, Lichen Planus is considered an autoimmune inflammatory disease. In autoimmune conditions, the immune system, which normally protects the body from infections and harmful substances, becomes overactive and targets healthy tissues. In the case of Lichen Planus, immune cells attack the skin or mucosal tissues, leading to swelling, redness, and the formation of characteristic rashes or patches. While the exact cause of this immune response is not completely understood, it is believed that certain triggers such as infections, medications, stress, or genetic predisposition may play a role.
Lichen Planus can affect multiple areas of the body, which is one reason why it can present with different symptoms. The most commonly affected areas include the skin, where purple or reddish bumps may appear on the wrists, ankles, lower back, or legs. It can also develop in the mouth, causing white streaks, patches, or painful sores known as oral lichen planus. In some individuals, the condition affects the scalp, potentially leading to hair loss, while others may experience changes in the nails, such as ridges, thinning, or nail damage. In certain cases, Lichen Planus may also affect the genital area, causing irritation or painful lesions.
The condition may occur as either acute or chronic. Acute cases usually appear suddenly and may resolve within several months to a year. Chronic cases, however, can last much longer and may require ongoing treatment to control symptoms and prevent flare-ups.
Lichen Planus can affect people of any age, but it is most commonly seen in middle-aged adults, particularly those between 30 and 60 years old. Certain forms, such as oral lichen planus, appear more frequently in women. People with autoimmune disorders or specific medical conditions may also have a slightly higher risk of developing this condition.
Lichen Planus Causes
The exact causes of Lichen Planus are not completely understood, but medical experts believe that several internal and external factors may contribute to its development. In most cases, the condition occurs when the body’s immune system becomes overactive and begins to attack healthy tissues in the skin or mucous membranes. This abnormal immune reaction leads to inflammation and the formation of characteristic lesions associated with the condition. While researchers continue to study the underlying mechanisms, multiple triggers and risk factors have been identified that may increase the likelihood of developing Lichen Planus.
Immune System Malfunction
One of the most widely accepted explanations for the development of Lichen Planus is an abnormal response of the immune system. Normally, the immune system protects the body by identifying and destroying harmful bacteria, viruses, and other foreign substances. However, in individuals with Lichen Planus, certain immune cells mistakenly target the body’s own skin or mucosal tissues. This immune attack results in inflammation and damage to the affected areas, which leads to the visible symptoms of the condition. Because of this mechanism, Lichen Planus is often categorized as an autoimmune-related inflammatory disorder.
Genetic Factors
Genetics may also play a role in increasing susceptibility to Lichen Planus. Although the condition is not directly inherited in most cases, some studies suggest that people with a family history of autoimmune disorders may have a higher risk of developing similar immune-related conditions. Certain genetic traits may influence how the immune system functions, making some individuals more prone to inflammatory responses. While genetics alone may not cause Lichen Planus, they can contribute to an increased vulnerability when combined with other triggers.
Viral Infections as Possible Triggers
Some research has indicated that viral infections may act as triggers for Lichen Planus in certain individuals. In particular, infections that stimulate the immune system may lead to an abnormal immune reaction that affects the skin or mucous membranes. Scientists have explored possible links between Lichen Planus and certain viral conditions, suggesting that infection-related immune responses could initiate the inflammatory process. However, this connection is still being studied, and viral infections are considered potential triggers rather than direct causes.
Allergic Reactions to Medications
Certain medications have also been associated with reactions that resemble or trigger Lichen Planus. Drugs used to treat conditions such as high blood pressure, heart disease, arthritis, and malaria have occasionally been linked to skin reactions similar to those seen in Lichen Planus. These reactions may occur when the immune system responds negatively to a medication or one of its ingredients. In some cases, symptoms may improve once the medication is discontinued under medical supervision.
Stress and Lifestyle Triggers
Psychological stress and lifestyle factors may contribute to flare-ups or worsening of symptoms in individuals with Lichen Planus. Chronic stress can weaken the body’s natural balance and affect immune function, potentially increasing inflammation in the body. Poor sleep, unhealthy diet habits, and excessive fatigue may also influence how the immune system responds to various triggers. While stress may not directly cause the condition, it is often recognized as a factor that can aggravate symptoms or trigger episodes in susceptible individuals.
Environmental Factors
Environmental influences may also play a role in the development or activation of Lichen Planus. Exposure to certain chemicals, allergens, or irritants can potentially provoke immune reactions in sensitive individuals. In some cases, dental materials, skin products, or contact with certain substances may irritate the skin or mucous membranes, contributing to inflammation. These environmental exposures may not cause the condition on their own, but they can act as contributing factors that trigger or worsen symptoms in people who are already predisposed to the disorder.
Risk Factors for Lichen Planus
Although Lichen Planus can develop in many individuals without a clear reason, certain factors may increase the likelihood of developing this inflammatory condition. These risk factors do not necessarily guarantee that someone will develop Lichen Planus, but they can make a person more susceptible to the disease. Understanding these factors can help individuals recognize potential risks and seek medical advice if symptoms appear.
Age Group Most Affected
Lichen Planus is most frequently diagnosed in middle-aged adults, particularly those between the ages of 30 and 60 years. While it can occur in younger individuals and older adults, it is relatively uncommon in children. The higher occurrence in middle-aged populations may be related to changes in the immune system or long-term exposure to environmental triggers and medications over time. Because the condition often appears during this stage of life, individuals within this age group should pay attention to unusual skin changes or persistent irritation.
Gender Differences
Both men and women can develop Lichen Planus, but some variations in occurrence have been observed. In general, the overall rate of the condition is fairly similar between genders. However, certain forms of the disease appear more frequently in women. For example, oral lichen planus, which affects the lining of the mouth, is reported more often in women than in men. Hormonal influences, immune responses, and lifestyle differences may contribute to these variations, although more research is needed to fully understand these patterns.
Family History
A family history of autoimmune or inflammatory conditions may also increase the risk of developing Lichen Planus. Although the disorder is not typically passed directly from parent to child, genetic factors may influence how the immune system reacts to triggers. Individuals who have relatives with autoimmune diseases may have a higher likelihood of experiencing immune-related disorders themselves. These inherited tendencies can make certain people more vulnerable to inflammatory conditions, including Lichen Planus.
Certain Medications
Some medications are known to trigger reactions that resemble Lichen Planus or may contribute to its development in sensitive individuals. Drugs commonly used to treat high blood pressure, heart conditions, arthritis, and certain infections have been linked to similar skin reactions in some patients. In these cases, the body may respond to the medication by producing inflammation that leads to symptoms resembling Lichen Planus. If a medication is suspected to be the cause, a healthcare provider may adjust the treatment plan or recommend alternatives.
Underlying Medical Conditions
Certain health conditions may also increase the likelihood of developing Lichen Planus. People who have autoimmune diseases, liver disorders, or chronic inflammatory conditions may have a higher risk. These underlying health issues can affect the immune system and may contribute to abnormal immune responses that lead to skin or mucosal inflammation.
Exposure to Chemicals or Allergens
Environmental exposures can sometimes act as triggers for Lichen Planus in susceptible individuals. Contact with certain chemicals, metals, dental materials, or allergens may irritate the skin or mucous membranes and stimulate an immune response. Repeated exposure to such substances may increase the chances of developing inflammation that contributes to the onset of the condition. Avoiding known irritants and maintaining good skin care practices can help reduce potential risks.
Lichen Planus Symptoms
The symptoms of Lichen Planus can vary widely depending on which part of the body is affected. Some people experience only mild skin irritation, while others may develop more noticeable lesions in the mouth, scalp, nails, or genital area. The condition often causes discomfort, itching, or inflammation, and in some cases the symptoms may persist for a long period. Recognizing these signs early can help individuals seek proper medical evaluation and treatment.
1. Skin Symptoms
The most recognizable signs of Lichen Planus appear on the skin. Individuals often develop small, purplish or reddish bumps that have a flat surface and a shiny appearance. These bumps may appear in clusters and are commonly found on the wrists, ankles, forearms, lower back, or legs. Over time, the bumps can spread and form noticeable rash patterns on the skin.
Another common feature is intense itching, which may range from mild to severe. Scratching the affected area can sometimes worsen irritation or lead to additional inflammation. After the rash heals, the skin may temporarily appear darker than the surrounding area, especially in people with darker skin tones.
2. Oral Symptoms (Oral Lichen Planus)
When the condition affects the mouth, it is known as oral lichen planus. This form usually appears as white, lace-like patches on the inside of the cheeks, tongue, gums, or lips. In some cases, the patches may look slightly raised or form thin lines across the mucous membrane.
Some individuals experience burning sensations, tenderness, or pain, particularly when eating spicy, acidic, or hot foods. In more severe cases, the inner lining of the mouth may develop ulcers or open sores, which can make speaking, eating, or drinking uncomfortable.
3. Nail Symptoms
Lichen Planus can also affect the nails, although this is less common. The condition may cause the nails to become thin, brittle, or fragile. Some people notice the development of long ridges or grooves on the nail surface. In severe cases, damage to the nail structure may lead to partial or complete nail loss if the inflammation affects the nail root.
4. Scalp Symptoms (Lichen Planopilaris)
When Lichen Planus involves the scalp, the condition is known as lichen planopilaris. This form can cause redness, irritation, and inflammation around the hair follicles. As the condition progresses, it may lead to hair thinning or hair loss in the affected areas. In some cases, the hair loss may become permanent if the follicles are severely damaged.
5. Genital Symptoms
Lichen Planus can also occur in the genital region, affecting both men and women. Symptoms may include painful lesions, redness, or sensitive patches on the genital skin. Some individuals experience burning sensations, itching, or discomfort, particularly during daily activities or sexual contact. Proper diagnosis and treatment are important to manage these symptoms effectively.
Types of Lichen Planus
Lichen Planus can appear in several forms depending on the part of the body involved. Each type has unique characteristics and may produce different symptoms. Some types mainly affect the skin, while others involve mucous membranes, hair follicles, or nails. Understanding the different types of Lichen Planus can help in identifying the condition and choosing the most suitable treatment approach.
1. Cutaneous Lichen Planus
Cutaneous Lichen Planus is the most common form of the condition and primarily affects the skin. It is usually recognized by clusters of purplish or reddish bumps that develop on areas such as the wrists, ankles, lower back, and legs. These bumps often have a flat surface and may appear shiny. The affected skin may also develop dark patches after the lesions heal. This type is frequently associated with itching and irritation.
2. Oral Lichen Planus
Oral Lichen Planus occurs inside the mouth and affects the mucous membranes. It commonly appears as thin white lines or lace-like patterns on the inner cheeks, tongue, or gums. In some cases, the affected tissue may become red, swollen, or sensitive. Certain individuals may experience discomfort while eating or drinking, especially when consuming spicy or acidic foods. This form of the condition may persist for long periods and often requires medical monitoring.
3. Lichen Planopilaris
Lichen Planopilaris is a type that affects the scalp and hair follicles. Inflammation develops around the hair roots, which can cause redness, irritation, and gradual hair thinning. Over time, the damage to hair follicles may lead to permanent hair loss in the affected areas if not managed properly.
4. Nail Lichen Planus
When the disorder involves the nails, it is known as nail lichen planus. This type can lead to structural changes in the nails, including ridges, grooves, thinning, or brittleness. In severe situations, the nail may separate from the nail bed or stop growing normally.
5. Hypertrophic Lichen Planus
Hypertrophic Lichen Planus is characterized by thick, raised skin lesions that often develop on the legs or ankles. These areas of skin may appear rough and may remain for a long time compared to other forms.
6. Erosive Lichen Planus
Erosive Lichen Planus is considered one of the more severe and painful forms of the condition. It often affects sensitive areas such as the mouth or genital region, where it can cause ulcers, raw patches, and significant discomfort. Medical treatment is usually required to control inflammation and relieve symptoms.
Lichen Planus Diagnosis
Diagnosing Lichen Planus involves a careful combination of medical evaluation, clinical examination, and sometimes laboratory tests. The process begins with a detailed medical history, where the doctor asks about the onset of symptoms, their duration, triggers, and any family history of autoimmune or inflammatory conditions. This step helps to identify patterns that may suggest Lichen Planus or related disorders.
A thorough physical examination follows, focusing on the affected areas of the body. The doctor inspects the skin, scalp, nails, mouth, and genital regions for characteristic lesions, patterns, or discoloration. Observing the shape, color, and distribution of bumps or patches provides essential clues for an accurate diagnosis.
In many cases, a skin biopsy is performed to confirm the condition. During this procedure, a small sample of the affected skin is removed and examined under a microscope. Histological analysis can reveal the specific type of immune response and cellular changes associated with Lichen Planus, helping differentiate it from other skin disorders.
Additional investigations may include blood tests to check for underlying autoimmune or systemic conditions that could be linked to the disease. These tests help evaluate overall health and rule out contributing factors such as liver disease or infections. Allergy testing may also be recommended if a reaction to medications, dental materials, or environmental triggers is suspected.
Finally, the doctor performs a differential diagnosis to distinguish Lichen Planus from other similar conditions, including eczema, psoriasis, fungal infections, or other oral and skin disorders. Correct diagnosis ensures appropriate treatment, reduces the risk of complications, and helps manage symptoms effectively.
Lichen Planus Treatment
Lichen Planus treament options focuses on reducing inflammation, relieving discomfort, and preventing complications. Treatment plans are tailored to the severity of the condition, the areas affected, and the patient’s overall health. While there is no permanent cure, a combination of medical therapies, topical applications, herbal supplements for Lichen Planus and lifestyle adjustments can significantly improve symptoms.
1. Medications
Various medications are used to control inflammation and suppress overactive immune responses. Corticosteroids are commonly prescribed to reduce swelling and irritation, either orally or as injections in more severe cases. Antihistamines can help manage intense itching and discomfort. Retinoids, derived from vitamin A, may be recommended for persistent skin lesions, particularly when conventional therapies are insufficient. In serious or widespread cases, immunosuppressants may be used to regulate the immune system and prevent further tissue damage.
2. Topical Treatments
For localized symptoms, topical therapies are often effective. Steroid creams are applied directly to the affected areas to minimize inflammation and itching. In addition, anti-inflammatory ointments can soothe irritated skin and support the healing process. These treatments are generally considered safe for short-term use but require monitoring when used over larger areas or for extended periods.
3. Light Therapy (Phototherapy)
Phototherapy, or controlled exposure to ultraviolet (UV) light, can be beneficial for extensive skin involvement. UV therapy works by modulating the immune response in the skin, reducing inflammation, and improving the appearance of lesions over time. Treatments are typically conducted in a clinical setting under professional supervision to avoid potential side effects.
4. Oral Treatments
In cases where Lichen Planus affects the mouth or becomes severe, oral medications may be necessary. These treatments help manage pain, decrease inflammation, and control persistent outbreaks that do not respond to topical therapies alone.
5. Natural & Home Remedies
Certain home-based strategies and remedies may complement medical treatment. Aloe vera can soothe irritated skin, while turmeric is valued for its anti-inflammatory properties. Reducing stress through mindfulness, meditation, or relaxation techniques may prevent flare-ups, and adopting a balanced diet rich in vitamins and antioxidants can support overall skin health. These approaches, while supportive, should be used alongside professional care for the best results.
Lifestyle and Diet Tips for Managing Lichen Planus
Adopting a healthy lifestyle and diet can play a supportive role in managing Lichen Planus and reducing flare-ups. An anti-inflammatory diet is often recommended, which includes plenty of fruits, vegetables, whole grains, and foods rich in omega-3 fatty acids, such as fatty fish, flaxseeds, and walnuts. These foods help lower systemic inflammation and may improve the overall condition of the skin and mucous membranes.
Certain foods and beverages should be avoided, particularly those that can irritate the mouth or trigger inflammation. Spicy, acidic, or heavily processed foods, as well as excessive caffeine or alcohol, may worsen oral or skin symptoms. Identifying personal triggers through observation can help minimize discomfort and prevent lesions from developing.
Maintaining proper oral hygiene practices is essential, especially for individuals with oral Lichen Planus. Gentle brushing, using soft-bristled toothbrushes, and rinsing with mild, non-alcoholic mouthwashes can prevent irritation and reduce the risk of secondary infections.
Stress management is another crucial factor. Chronic stress may exacerbate immune system imbalances, so incorporating relaxation techniques, meditation, deep-breathing exercises, or regular physical activity can help control symptoms.
Lastly, a consistent skin care routine can support affected areas. Using mild, fragrance-free cleansers, moisturizing regularly, and avoiding harsh soaps or detergents helps maintain skin integrity and reduce irritation, complementing medical treatments effectively.
Possible Complications
While Lichen Planus is generally not life-threatening, it can lead to several complications if left unmanaged or if symptoms become severe. One of the most common issues is chronic pain, which may result from persistent itching, irritation, or the development of sores on the skin or mucous membranes. This ongoing discomfort can affect daily activities, sleep quality, and overall quality of life.
Another frequent complication is skin discoloration. Even after lesions heal, the affected areas may remain darker or lighter than surrounding skin, creating lasting cosmetic concerns. These changes can be particularly noticeable in individuals with darker skin tones and may contribute to self-consciousness or emotional distress.
When Lichen Planus involves the scalp, known as lichen planopilaris, it may lead to hair loss. In some cases, inflammation damages hair follicles permanently, resulting in patchy or permanent bald spots. Similarly, nail involvement can cause ridging, thinning, or splitting, and in severe cases, nails may become deformed or partially lost, which can impact daily tasks and hand function.
In rare instances, individuals with oral Lichen Planus may experience an increased risk of developing oral cancer. This risk is relatively low, but persistent or worsening lesions in the mouth should always be evaluated promptly by a healthcare professional. Regular dental checkups and monitoring of oral lesions are essential for early detection of potential malignancies.
Although complications vary depending on the type and severity of Lichen Planus timely diagnosis and appropriate management can significantly reduce these risks. Following medical advice, maintaining good oral and skin care practices, and addressing flare-ups early are key strategies to prevent long-term problems and maintain overall health.
Lichen Planus Prevention
Although Lichen Planus cannot always be completely prevented, certain measures can reduce the likelihood of flare-ups and help manage the condition effectively. One of the most important strategies is to avoid known triggers. These can include specific medications, allergens, or foods that irritate the skin or mucous membranes. Keeping a diary of symptoms and potential triggers can help identify and minimize exposure to these factors.
Stress management is another key preventive measure. High levels of stress can disrupt immune system balance and contribute to inflammation. Incorporating relaxation techniques, such as yoga, meditation, deep-breathing exercises, or regular physical activity, can help maintain emotional well-being and reduce the risk of symptom exacerbation.
Maintaining a healthy immune system through proper nutrition, adequate sleep, and regular exercise also supports the body’s ability to manage inflammation. A diet rich in vitamins, minerals, and antioxidants can enhance overall skin and mucosal health, while avoiding excessive alcohol or processed foods may prevent immune system overload.
It is equally important to avoid irritating products. Harsh soaps, fragranced skincare items, and abrasive dental products can worsen inflammation or cause additional discomfort. Choosing gentle, hypoallergenic options can protect the skin and oral tissues while supporting healing.
Finally, regular medical checkups play a critical role in prevention. Routine visits allow healthcare providers to monitor existing lesions, detect early signs of complications, and adjust treatment plans as needed. Consistent medical follow-up ensures that any changes in the condition are addressed promptly, reducing the risk of severe outbreaks or long-term damage.
By combining these preventive strategies, individuals with Lichen Planus can better control symptoms, minimize flare-ups, and maintain a higher quality of life.
When to See a Doctor
It is important to seek medical attention for Lichen Planus when symptoms persist or interfere with daily life. A rash that does not improve after a few weeks of self-care should be evaluated by a healthcare professional to rule out other skin conditions and confirm a proper diagnosis.
Painful sores or patches in the mouth that make eating, drinking, or speaking uncomfortable also warrant a medical visit. Early intervention can reduce discomfort and prevent complications such as secondary infections or ulceration.
If you notice hair loss or thinning in localized areas of the scalp, professional assessment is necessary to prevent permanent follicle damage. Similarly, changes in the nails, including splitting, ridging, or nail loss, should be monitored to maintain nail health.
Finally, any symptoms that interfere with daily activities, such as severe itching, pain, or difficulty performing routine tasks, require prompt consultation. Early diagnosis and appropriate treatment can manage symptoms effectively and reduce the risk of long-term complications.
Frequently Asked Questions (FAQs)
Is Lichen Planus contagious?
No, Lichen Planus is not contagious. Can lichen planus spread? No, it cannot spread from one person to another through physical contact, sharing food, or using the same personal items. It is an inflammatory condition that occurs when the immune system mistakenly attacks the skin or mucous membranes.
How long does Lichen Planus last?
The duration of Lichen Planus varies from person to person. In many cases, skin Lichen Planus may clear within 1–2 years, while oral Lichen Planus can last longer and may come and go over time. Proper treatment and lifestyle changes can help manage symptoms and reduce flare-ups.
Can Lichen Planus be cured permanently?
There is currently no guaranteed permanent cure for Lichen Planus, but many treatments can effectively control the condition and relieve symptoms. With proper medical care, good oral hygiene, and avoiding triggers, many people experience long periods without symptoms.
Is Lichen Planus dangerous?
Lichen Planus is generally not life-threatening. However, it can cause discomfort, itching, or painful mouth sores. In rare cases, long-standing oral Lichen Planus may slightly increase the risk of oral cancer, which is why regular medical checkups are recommended.
What foods trigger Lichen Planus?
Certain foods may worsen symptoms, especially in oral Lichen Planus. Common triggers include spicy foods, acidic fruits (like citrus), salty snacks, alcohol, and very hot beverages. Avoiding irritating foods and maintaining a balanced diet can help reduce flare-ups.
Conclusion
Lichen Planus is a long-lasting inflammatory disorder that can affect different parts of the body, including the skin, mouth, scalp, nails, and genital area. Throughout this article, we explored how the condition develops due to an abnormal immune response and how various factors such as genetics, medications, infections, stress, and environmental triggers may contribute to its onset. The discussion also highlighted the different forms of the disease, common symptoms, possible complications, and the methods used by healthcare professionals to identify it.
Recognizing the condition at an early stage is very important. Timely identification of unusual rashes, persistent mouth lesions, nail changes, or scalp irritation allows healthcare providers to evaluate the problem before it progresses or leads to long-term complications. Early assessment can also help distinguish Lichen Planus from other skin or oral disorders that may appear similar.
A variety of management options are available to help control symptoms and improve quality of life. These include prescription medications, topical therapies, light-based treatments, and supportive lifestyle changes such as maintaining good skin and oral care, managing stress, and following a balanced diet. Although the condition may not always disappear permanently, proper treatment can significantly reduce inflammation, discomfort, and flare-ups.
Anyone experiencing ongoing itching, unusual rashes, mouth sores, or other persistent symptoms should not ignore them. Consulting a qualified healthcare professional ensures accurate diagnosis and appropriate care. Seeking medical advice early can lead to better symptom control and help prevent potential complications in the future.