Achalasia is a rare but serious condition affecting the esophagus — the muscular tube that connects your throat to your stomach. Although it is not always life-threatening by itself, achalasia complications can be significant, chronic, and in some cases dangerous if the condition is not treated effectively or monitored over time. Understanding what achalasia is and the risks associated with it is crucial for patients, caregivers, and anyone seeking to learn about the long-term impacts of the disease.
What Is Achalasia? A Quick Overview
Achalasia is a chronic disorder of the esophagus characterized by the loss of normal nerve function in the esophageal muscles and failure of the lower esophageal sphincter (LES) to relax properly during swallowing. This results in difficulty moving food and liquids from the esophagus into the stomach. Food can accumulate in the esophagus, leading to discomfort, regurgitation, and other symptoms. There is no cure, but treatments aim to improve swallowing and reduce pressure at the LES.
The condition is rare, typically affecting adults between ages 25 and 60, but it can occur at any age. Because symptoms often develop slowly and mimic other digestive disorders like gastroesophageal reflux disease (GERD), diagnosis may be delayed.
How Dangerous Is Achalasia?
Achalasia itself is not usually immediately life-threatening for most people — particularly those who receive prompt and appropriate treatment — but it is a serious medical condition with potential long-term consequences. Without treatment, achalasia complications can accumulate and worsen over time, impacting health, quality of life, nutrition, and even lifespan.
Common and Serious Complications of Achalasia
Here’s a focused look at key complications that can occur with achalasia, especially when the condition goes untreated or progresses.
1. Dysphagia: Difficulty Swallowing
The hallmark symptom of achalasia is dysphagia — difficulty swallowing solids and liquids. Dysphagia occurs because the esophageal muscles lose coordinated function and the LES fails to relax properly, making it hard for food to pass into the stomach. This symptom typically worsens over time and can lead to frustration, discomfort, and potential nutritional deficits if not managed.
Long-term retention of food in the esophagus increases the risk that food will ferment or decompose, leading to irritation and further complications.
2. Regurgitation and Aspiration
One of the most concerning achalasia complications is regurgitation — the backward flow of undigested food and saliva. Unlike typical acid reflux, this regurgitation is food that never reached the stomach. When regurgitated material enters the airways during sleep or while eating, it can cause aspiration, which is when food or liquids are inhaled into the lungs.
This can lead to:
- Aspiration pneumonia
- Chronic lung inflammation
- Bronchiectasis and other pulmonary issues
Aspiration pneumonia can be particularly dangerous in older adults or people with weakened immune systems, and it may require antibiotics or hospitalization.
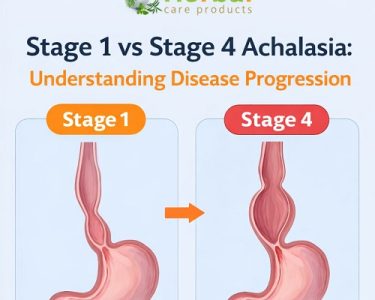
3. Esophageal Dilation and Megaesophagus
When food and liquids remain in the esophagus for long periods, the esophagus can stretch and lose strength. Over time, the esophagus can become significantly enlarged — a condition called megaesophagus. This dilation worsens achalasia complications, making it even harder to swallow and decreasing the effectiveness of treatments. A widened or “baggy” esophagus can develop tortuosity (twisting), leading to further swallowing issues and discomfort.
Megaesophagus also increases the risk of food stasis and inflammation — a dangerous cycle that feeds into other complications.
4. Esophagitis: Irritation of the Esophagus
Food and fluid that sit in the esophagus too long can irritate the lining, causing inflammation known as esophagitis. This is a significant achalasia complication because ongoing irritation can damage esophageal tissue and heighten the risk of other issues like ulcers or bleeding. Inflammation can also worsen dysphagia and discomfort.
5. Esophageal Perforation
Although rare, one serious complication of both untreated achalasia and certain treatments (like pneumatic dilation or surgery) is esophageal perforation — a hole or tear in the wall of the esophagus. Perforation is a medical emergency that can lead to severe infection and requires immediate attention. Symptoms may include sudden chest pain, fever, rapid heart rate, and severe difficulty swallowing.
6. Malnutrition and Weight Loss
Ongoing difficulty swallowing and loss of appetite can lead to unintentional weight loss and malnutrition. When your body cannot properly take in food and nutrients, muscle mass, energy levels, and immune function can decline. Chronic malnutrition is a dangerous condition that can affect multiple organ systems, reduce life expectancy, and make infections or other illnesses more serious.
This can also contribute to fatigue and physical weakness, affecting daily functioning and quality of life.
7. Post-Treatment Reflux and Barrett’s Esophagus
After certain treatments designed to weaken or cut the LES — such as pneumatic dilation, surgical myotomy, or peroral endoscopic myotomy (POEM) — some patients experience gastroesophageal reflux (GERD). Reflux occurs when stomach acid backs up into the esophagus.
Chronic reflux can irritate the esophageal lining and, in some cases, lead to Barrett’s esophagus, a condition where the lining of the esophagus changes and becomes similar to the intestinal lining. Barrett’s esophagus is considered a precancerous change and increases the risk of esophageal adenocarcinoma.
Reflux after achalasia treatment is one of the recognized achalasia complications that patients and clinicians monitor closely.
Long-Term Risk of Esophageal Cancer
Perhaps the most serious long-term concern with achalasia is an increased risk of esophageal cancer.
Esophageal Squamous Cell Carcinoma (ESCC)
In patients with chronic achalasia, especially longstanding, untreated disease, studies have shown a much higher risk of esophageal squamous cell carcinoma compared to the general population. Estimates vary substantially, but some research suggests risks anywhere from 16 times to up to 50 times higher than average — particularly after many years of untreated food stasis and mucosal irritation.
The mechanism is thought to be chronic inflammation and irritation of the esophageal mucosa due to retained food and bacterial fermentation. Tissue changes over time can lead to precancerous dysplasia and eventually malignancy.
Esophageal Adenocarcinoma
While ESCC is more strongly associated with achalasia, adenocarcinoma can also develop — especially when achalasia patients develop Barrett’s esophagus after treatment-related reflux.
Endoscopic Surveillance
Because of these risks, some experts recommend routine endoscopic surveillance with tissue sampling to detect early changes or precancerous lesions, especially in patients with longstanding achalasia (e.g., 10–15+ years of disease). Although guidelines are not universally standardized, many clinicians incorporate periodic surveillance into long-term management plans.
Other Long-Term Health and Quality-of-Life Issues
In addition to the major medical complications already discussed, achalasia can affect overall well-being in other ways.
Chronic Chest Pain and Discomfort
Pain and discomfort from esophageal stretching, spasm, or retained food can be ongoing. This contributes to anxiety, altered eating behaviors, and reduced quality of life. Some patients adjust their diets drastically to manage symptoms.
Psychological and Social Impact
Living with a chronic condition like achalasia can contribute to stress, anxiety, and depression. Social activities involving eating can become challenging, and patients may avoid social dining to prevent embarrassment or discomfort.
Recurrent Treatments and Follow-Up
Achalasia treatments — whether surgical, endoscopic, or pharmaceutical — often require ongoing management. Some patients need repeat procedures because symptoms can return. Even after successful treatment, regular follow-up is necessary to monitor for complications like reflux, stricture development, or signs of malignancy.
Can Achalasia Be Fatal?
While achalasia itself is not usually a direct cause of death, the complications associated with it can be serious and, in rare cases, life-threatening — especially if left untreated:
- Aspiration pneumonia can be dangerous or fatal, particularly in older or immunocompromised adults.
- Esophageal perforation is a medical emergency and can lead to severe infection if not treated promptly.
- Severe malnutrition weakens the body’s defenses and worsens outcomes in other illnesses.
- Esophageal cancer is a serious malignancy with variable prognosis depending on stage at diagnosis.
With appropriate medical care, regular follow-up, and attention to symptoms, most people with achalasia can manage their condition and avoid the most severe outcomes. Early diagnosis and treatment are key elements in reducing the risk of serious complications.
How to Reduce Risks and Manage Complications
While achalasia cannot be cured, the risks and achalasia complications can often be minimized with a thoughtful treatment plan.
1. Seek Early Medical Evaluation
If you have symptoms like persistent difficulty swallowing, chronic regurgitation, or unexplained weight loss, seeing a gastroenterologist early can lead to timely diagnosis and treatment.
2. Treatment Options
Treatment approaches for achalasia focus on reducing pressure at the LES so food can pass into the stomach more easily:
- Pneumatic dilation
- Heller myotomy (surgical LES muscle cutting)
- Peroral Endoscopic Myotomy (POEM)
- Medications (limited but sometimes helpful)
- Botulinum toxin injections
Each option carries potential benefits and risks, and the best choice depends on the individual patient’s condition, age, and preferences.
3. Monitor and Manage Acid Reflux
Because treatments that reduce LES pressure can increase gastroesophageal reflux, managing reflux with lifestyle changes or medications is often important to prevent further irritation or Barrett’s esophagus.
4. Regular Follow-Up Care
Follow-up visits with endoscopic or imaging assessments help monitor for structural changes, complications, or early signs of malignancy — especially in long-term achalasia.
5. Dietary Modifications
Eating smaller, softer meals and chewing thoroughly helps food pass more easily. Some patients benefit from adjusting eating times, avoiding certain foods, and staying upright during and after meals.
Conclusion
Achalasia is a chronic esophageal motility disorder that can cause significant challenges over time. Although it is not immediately life-threatening for most people, achalasia complications — ranging from aspiration pneumonia and severe malnutrition to esophageal dilation and cancer — are serious and require careful medical attention.
With early diagnosis, appropriate treatment, ongoing surveillance, and lifestyle adjustments, many patients can live well for years with achalasia and reduce their risk of long-term complications. Awareness of the possible risks and proactive management is the cornerstone of healthier living with this condition.